9 Effective Pain Treatments That Aren’t Opioids, According to Doctors
January 31, 2019 by Steven M. PetersOften, our body’s way of telling us something is wrong is through pain — and this is a major reason for visiting the doctor. The problem is not always easily solved, however, and many people suffer from chronic pain.
Between 8% and 12% of chronic pain patients who are prescribed opioids will develop dependency on painkillers. Opioid addiction has become an epidemic in the United States. In 2017, more than 47,000 Americans died from opioid overdose, according to the National Institute on Drug Abuse. This is, on average, 128 deaths a day.
About 17,000 of these annual deaths involved opioids prescribed for treatment of moderate-to-severe pain (the rest are ascribed primarily to illegal street drugs).
Research has shown that instead of turning to powerful drugs, more than 50% of people with chronic musculoskeletal pain have sought out alternative treatments, with chiropractic care, massage, and acupuncture the most commonly used, according to Dr. Jonathan Koning, a board-certified pain management specialist and anesthesiologist.
“[For] most chronic pain conditions, like low back pain, neck pain, and fibromyalgia, complementary medical interventions have shown to improve pain levels, lessen depression, and improve functionality in some people.”
To identify some of the best available alternative pain treatment, 24/7 Wall St. consulted anesthesiologists and reviewed research in publications such as The Journal of the American Medical Association and Journal of Medical and Biological Engineering.
There’s a growing consensus nowadays that lifestyle changes need to be implemented in all chronic pain conditions, Koning noted. “And there’s a growing emphasis on these changes as opposed to hastily starting patients on medications.” The American College of Physicians, for example, updated its low back pain guidelines in 2017, suggesting doctors prescribe alternative therapies that don’t involve pills before opioids.
Over-the-counter medications, which are less potent and thus less addictive, may do the trick, too. One study of more than 400 emergency room patients with acute pain (which usually comes on suddenly, is caused by a specific incident, and doesn’t last long) from bone fractures, dislocated shoulders, and other injuries or conditions showed that OTC medicine was just as effective as opioids after two hours.
Some studies have shown that non-pharmaceutical interventions such as exercise, stress reduction and better diet can also be effective for some chronic pain patients.
Click here to see the 9 alternative pain treatments that aren’t opioids, according to doctors.
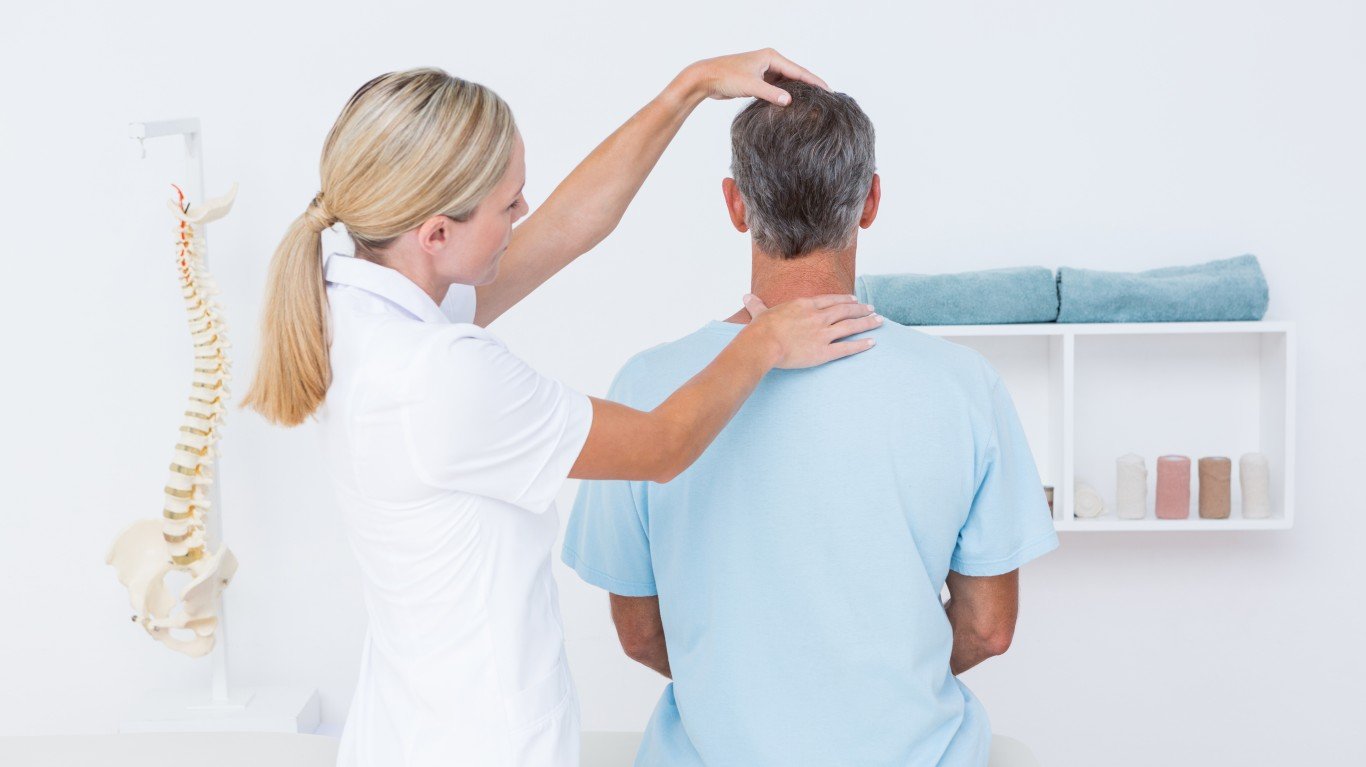
1. Chiropractic care
Koning says he refers many patients for chiropractic care. “There’s more to it than just ‘cracking and popping.'” Chiropractors can provide manual therapy, massage, stretching, and cervical or lumbar traction, which are helpful in alleviating muscle pain and improving range of motion and flexibility, he noted.
However, there are instances when chiropractic care should be avoided. This is “typically why I ask patients to consult with me before seeking chiropractic care,” Koning said. “I would not recommend this to patients with pain related to severe degenerative joint disease or spinal stenosis, for example.”
[in-text-ad]

2. Massage
After chiropractic treatment, massage is the most sought after treatment for chronic neck and low back pain, according to Koning. “It’s a mainstay for me in treating most of my patients.” Specifically, he recommends “lighter” pressure types, such as Swedish massage, for those with hypersensitivity syndromes like fibromyalgia, and for some with chronic headaches or migraines.
“Alternatively, for patients with chronic low back and neck pain, deep tissue [massage] can be more helpful over the long haul,” Koning said. If a patient is developing a lot of areas of focal muscle spasm, then the “stronger” myofascial release and deep tissue massages will more effectively treat them, he noted. But if a patient “hurts all over” and is very sensitive to touch, deep tissue isn’t going to help and may in fact worsen their pain, according to Koning. “So I recommend ‘lighter’ massage types like Swedish.”
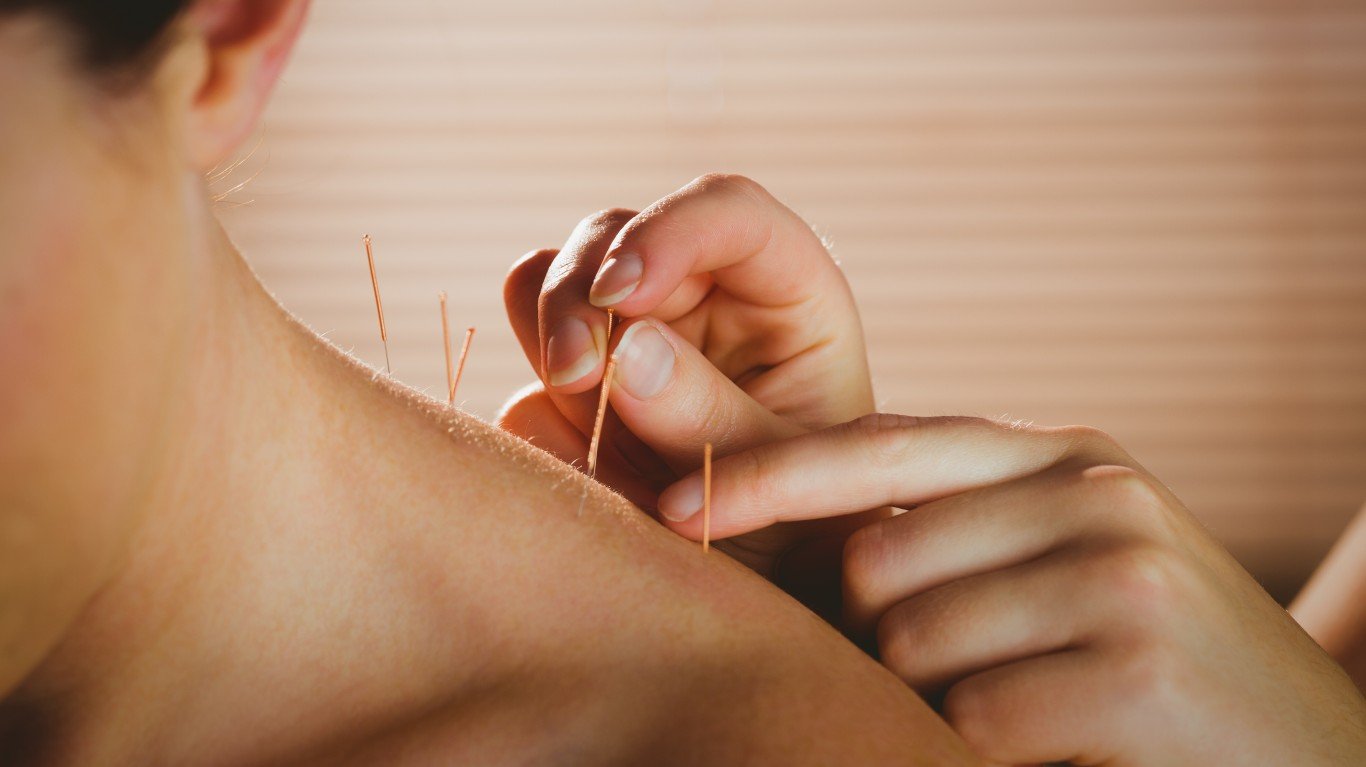
3. Acupuncture
“I think acupuncture has a place in pain management, but it doesn’t work in all cases, and the research on its efficacy is very conflicting,” Koning said. Some studies suggest it’s most effective in alleviating chronic neck pain and headaches. “I’ve found [this] anecdotally to be true, and will encourage patients with those problems to try it.” Also, it can be effective in improving low back pain, and one study recently even suggested its use in uncontrolled pain related to menstrual cramps, he noted.
“In all, acupuncture usually isn’t my first or second choice in alternative treatment options for patients.” Doctors are not sure quite how or if acupuncture works, he added. “We assume it works somehow by stimulating the body’s natural healing and anti-inflammatory reactions.”

4. Low-impact exercise
“Fibromyalgia is one of these chronic pain conditions in which the literature has suggested, recently, that plain old consistent low-impact exercise — such as walking, swimming, and cycling — is just as effective in reducing pain levels and increasing functionality as is taking opioids or anti-depressants,” Koning said. “In fact, in the case of fibromyalgia, taking opioids on a long term basis can actually worsen the progression of the disease over time, thus increasing instead of decreasing pain levels.”
[in-text-ad-2]

5. Yoga, Tai Chi, and Pilates
Yoga, tai chi, and Pilates have all been shown to be effective in improving pain scores and reducing stress, according to Koning. “I recommend this to most of my patients with chronic neck and low back pain, as well as chronic joint pain.”
Most studies will at least say that these practices are “not inferior” to other prescription medications, he noted. All of these practices involve slow, controlled body movements, which can over time strengthen muscles, shed weight, and improve balance in a way that reduces pain. “They also encourage mindfulness and meditation that can help switch one’s mind off of constantly thinking about pain,” Koning said.

6. Guided imagery
Guided imagery involves focusing the mind on pleasant and positive thoughts that can evoke strong positive emotions. It’s the equivalent of taking a mental vacation, or daydreaming, but in a very focused way, according to Koning. “It is primarily for stress reduction, but most chronic pain conditions can impose a significant level of stress, so it’s helpful in those cases as well.”
[in-text-ad]

7. Biofeedback
Biofeedback is learning to control what normally are involuntary functions. “It takes practice, and though some try to downplay it, it’s not at all a bogus treatment option,” Koning said. “It may be easier than you think.” One example is sitting down quietly and breathing deeply in and out for a minute. You’ll notice your heart rate will decrease, Koning noted.
Some studies have shown that cognitive-behavioral therapy and biofeedback, which teach someone how to emotionally adjust to the pain and meditate to manipulate the body’s physical reaction to pain, can be effective in reducing pain levels if practiced regularly, according to Koning.

8. Nutritional supplements
Natural herbs and spices like turmeric, cumin, and cayenne have shown to decrease inflammation when eaten regularly, and Koning recommends them all the time. “Magnesium, vitamin D, and B vitamins, and alpha-lipoic acid can be helpful in patients with restless leg syndrome, fibromyalgia, peripheral neuropathy, and insomnia,” Koning said. “Turmeric, cumin and glucosamine-chondroitin have been shown to help decrease pain related to degenerative joint disease.” Magnesium can also decrease migraine frequency, muscle spasms in patient with fibromyalgia, and chronic neck and back pain, he noted.
However, the problem with nutritional supplements is that it’s difficult to guarantee that you’re getting what you pay for, he added, because they are not subject to the same safety rules as drugs. Also, he noted, some supplements can be harmful when taking in excess. “It’s best to consult a physician about any supplements.”
9. Stem cell-based therapy
Stem cells can self-renew and replicate into certain other types of cells such as muscle or nerve cells. Stem cell-based therapy, or regenerative stem cell therapy, involves getting cells from one’s own bone marrow tissue or fat and injecting it back into the area of the body that hurts, such as a knee, shoulder, joint, or tendon. The treatment can be used instead of surgery or after to treat tissue pain, according to Dr. Michael Phillips, a pain medicine specialist in Arlington, Texas.
While there are high hopes for the future of stem cell-based therapies, the treatment is currently not FDA approved and potentially dangerous. The FDA recently issued a warning about unapproved stem cell treatments. Some clinics advertise the use of stem cells in their therapies, but are using amniotic fluid with no stem cells. “They are not regulated well enough, which opens the door to a lot of scams,” Phillips said.
Even the safest procedures are not for everyone. For example, it is not appropriate for people undergoing chemotherapy or taking certain medications, Phillips noted.
Sponsored: Find a Qualified Financial Advisor
Finding a qualified financial advisor doesn’t have to be hard. SmartAsset’s free tool matches you with up to 3 fiduciary financial advisors in your area in 5 minutes. Each advisor has been vetted by SmartAsset and is held to a fiduciary standard to act in your best interests. If you’re ready to be matched with local advisors that can help you achieve your financial goals, get started now.