Are All Insulin Pens Created Equal?
January 31, 2019 by Steven M. PetersNine percent of Americans, about 30 million people, have diabetes, according to the Centers for Disease Control and Prevention. About a fourth of them do not even know they have diabetes. Approximately 1.5 million people in the country are diagnosed with it each year.
Globally, between 400 million and 500 million people carry the disease, according to the CDC, and the number is increasing. In the United States, diabetes disproportionately affects minorities and is the sixth leading cause of disease-related death, claiming more than 80,000 people annually.
Some with Type 2 diabetes can reach their target blood sugar levels through diet and exercise. Others, however, may require a lifetime of doctor-prescribed, self-administered treatment such as insulin therapy. For decades in the 20th century, the only way to self-administer insulin was by traditional vial-and-syringe injections, which is still the most common form of delivery. About 20 years ago, however, drug companies began developing insulin pens, and today they are a popular (though more costly) alternative.
24/7 Wall St. examined news articles, product description documents from insulin pen manufacturers, and information provided by independent advocacy groups and government health agencies to create a list of 10 factors to consider before buying an insulin pen.
It is important to note that this list is to provide information and should not be used to self-diagnose dosages or insulin treatments. Always consult with your doctor before considering any changes to an existing regimen.
Click here to see if all insulin pens are created equal.
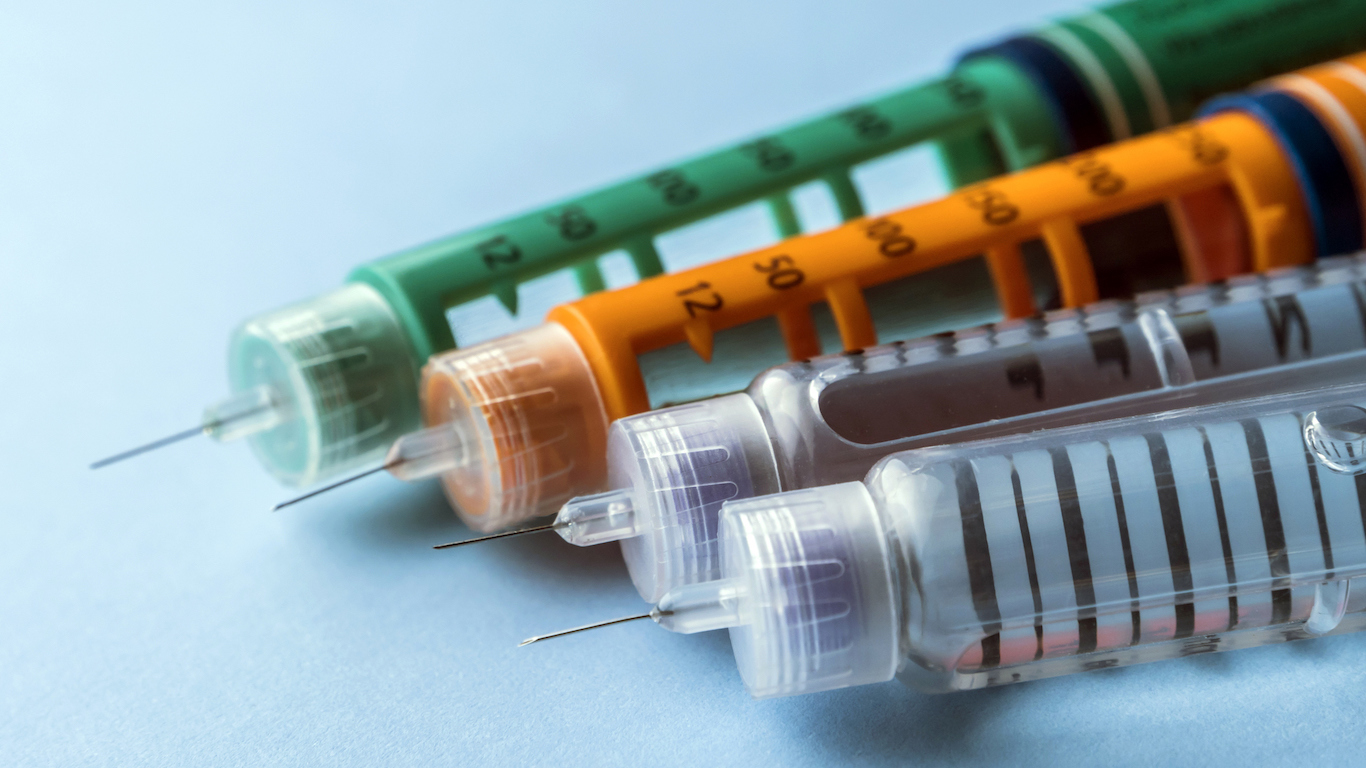
1. Capacity
The U.S. Food and Drug Administration approved last year a prefilled disposable long-acting insulin pen with the highest capacity yet, made by Sanofi. The device holds 900 units. What does that mean? Insulin is administered in unit increments. The recently approved insulin pen can provide up to 160 units per millimeter in a single injection, and may reduce the number of injections for adults with diabetes. Most insulin pens deliver up to 60 or 80 units per injection, adjustable in one-unit increments. They typically have capacities of 300 to 600 units. Depending on the patient, therefore, the number of injections or doses in insulin pens can vary. Many patients wind up requiring 30 units per injection.
[in-text-ad]
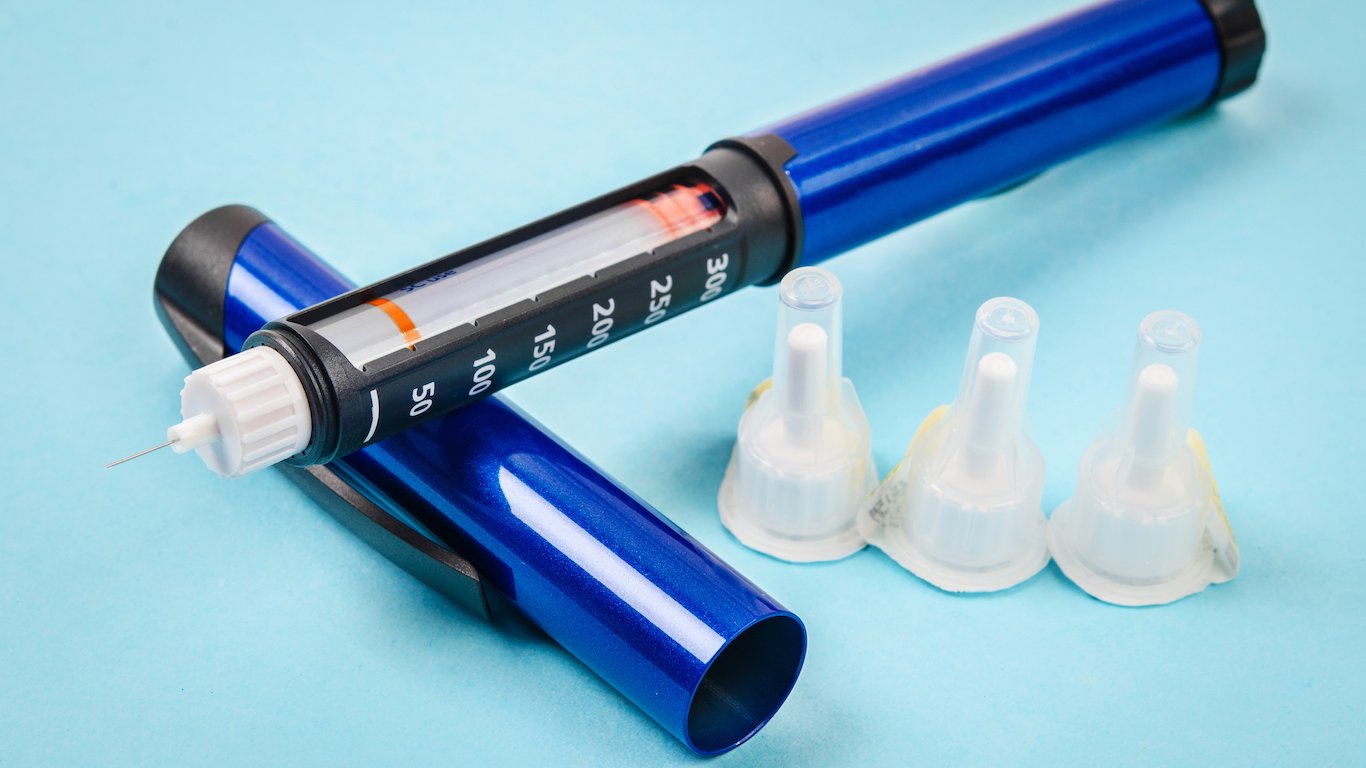
2. Color/style
There are many colors and styles of insulin pens, but they all more or less follow the same design guidelines. At a glance, an insulin pen could easily be mistaken for a large permanent marker because it has a shirt-pocket clip and a cap that protects the needle. (Needles are sold separately.) Major insulin pen makers develop and market pens with different types of insulin, so they typically use color and shape to indicate the type and brand of insulin the pen contains. If you do not like the way an insulin pen looks, it is possible to find a different color or style manufactured by another company that produces a comparable product. But options are limited.

3. Doses
The amount of insulin a patient needs depends on his or her specific condition. Doses are adjustable in insulin pens by using their “dial-a-dose” feature, typically measured in one-unit increments. Insulin pens contain 3 milliliters of insulin but the concentration of insulin varies. When someone suffering from Type 2 diabetes begins using insulin, it is common to start with a small dose and increase it incrementally until an ideal dose is achieved. Many people with Type 2 diabetes will start with 1 to 2 units of insulin for every kilogram (2.2 pounds) of body weight. A person weighing 176 pounds, for example, might start with one 12-unit injection per day.
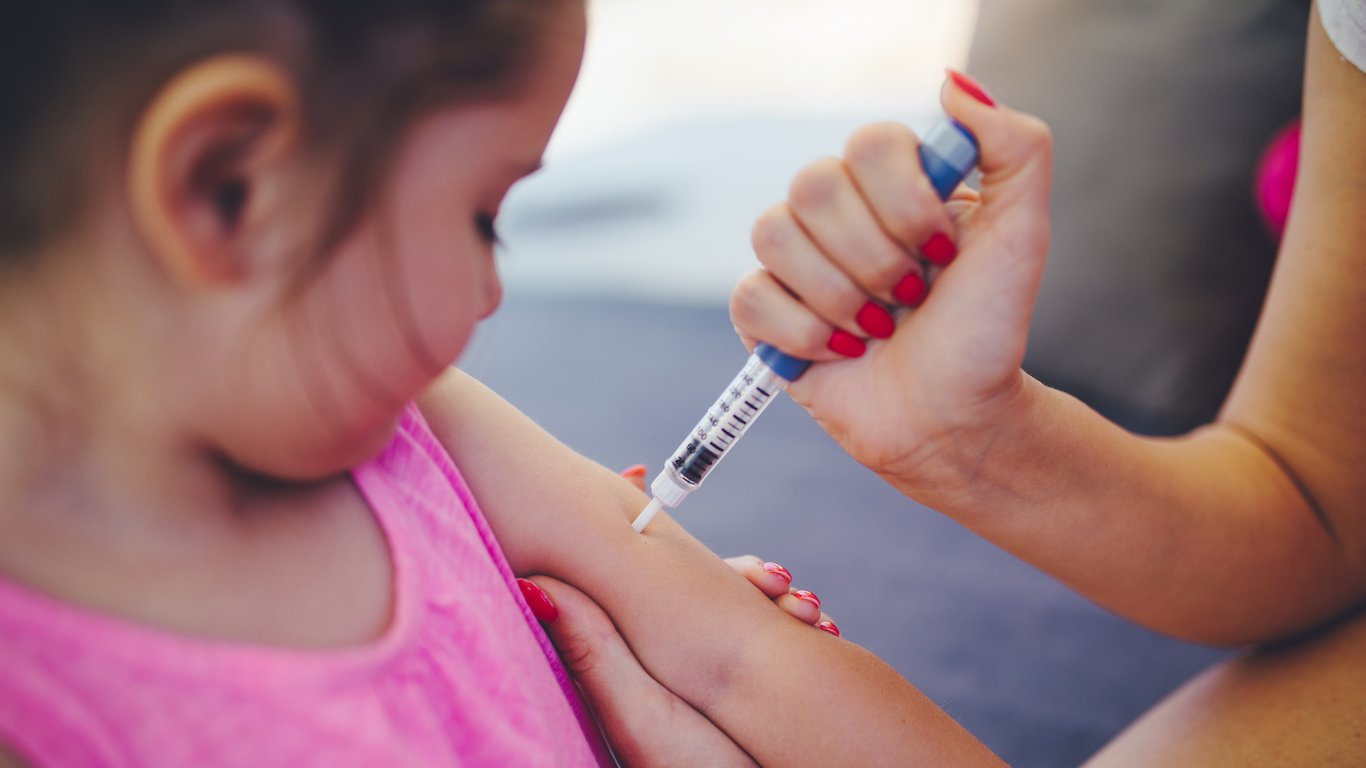
4. Needle length
One of the biggest issues for diabetics is that they have to self-administer injections, typically on a daily basis and often more than once per day. Insulin pens are designed to make this as painless and easy as possible, replacing the old-fashioned needle-and-syringe routine, which is not only cumbersome but also a challenge for patients who lack hand-eye coordination, such as the elderly. Needles, which are sold separately from insulin pens, come in different lengths, from 4 millimeters to 12.7 millimeters. The shorter needles work best for most adults and children, but consult with your doctor about what length works best for your specific needs because needle length can affect blood sugar control.
[in-text-ad-2]

5. Needle gauge
Another factor to consider with insulin pen needles (which are sold separately) is the gauge, or thickness. A thinner needle tends to mitigate the discomfort of injection. However, a thicker needle delivers the insulin dose more quickly. Needles should not be used more than once due to risk of infection. Doctors typically prescribe the needle along with the insulin, but it does not hurt to ask if you are being prescribed the shortest and thinnest needle possible for your specific needs. Also remember that when discussing needle gauge, the smaller the number the thicker the needle. Insulin pen needle gauges range from 29 to 33.
6. Manufacturers
The most popular insulin pens are designed and manufactured by the top three insulin suppliers â Denmark-based Novo Nordisk, Sanofi of France, and Indianapolis-based Eli Lilly. Together, these three companies had more than $29 billion in global revenue from diabetes treatments in 2018, according to pharmaceutical industry organization IgeaHub, more than half of the total revenue of the top 10 companies. The large influence these three companies have on the marketplace has led to criticisms about the recent steep increases in insulin prices, which jumped 300% from 2002 to 2013, according to a congressional report released late last year.
[in-text-ad]
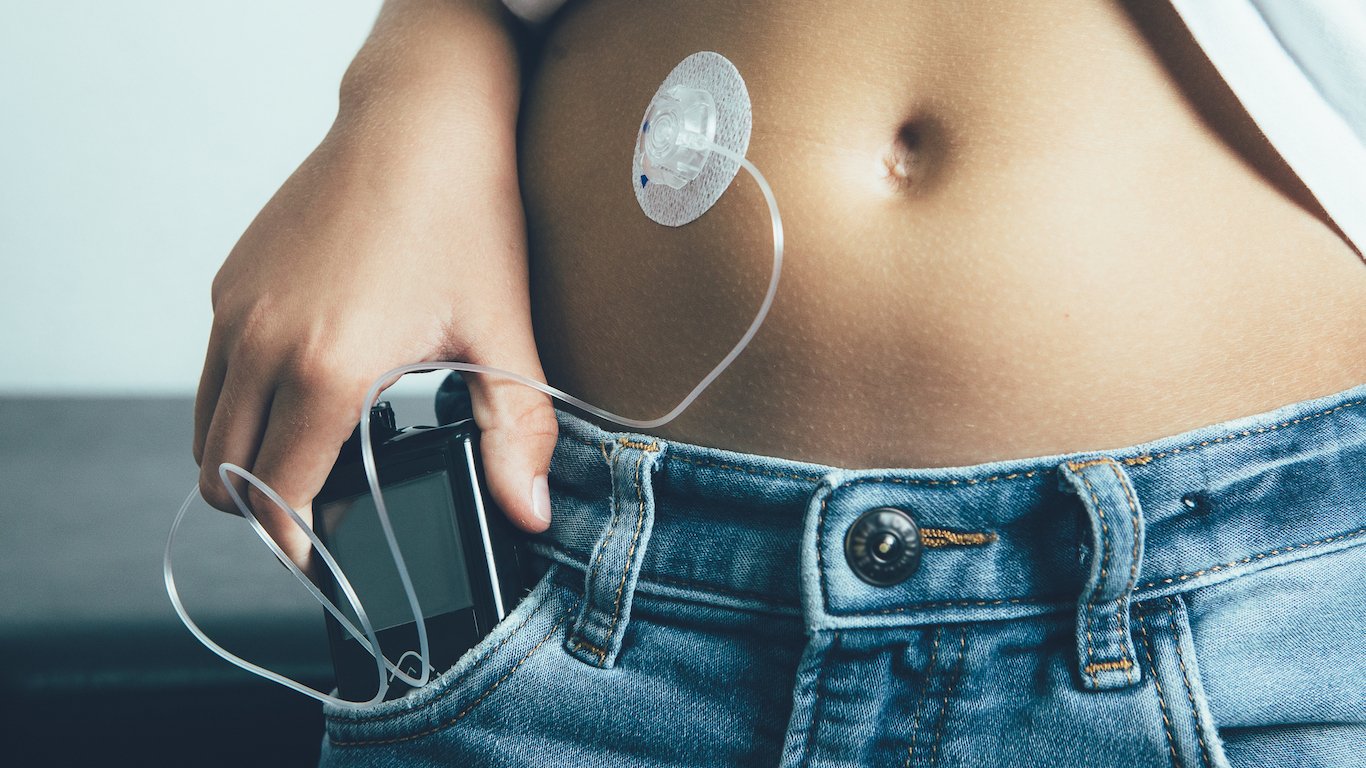
7. Pen Alternatives
Insulin pens are a more convenient way to inject insulin, but they are also more expensive than the traditional vial-and-syringe system, which therefore remains the most common way to inject insulin. The traditional system costs less but the injections can be more painful, more complicated to administer, and require users to carry around vials and syringes. Computerized insulin pumps, which are automated devices connected to infusion sets attached to the body, are becoming more common, but they cost thousands of dollars. Pumps may require special and costly in-patient training and are either not covered by insurance or covered under strict bureaucratic guidelines.

8. Pricing
Insulin pens cost more than vials and syringes. Syringes cost between $15 and $20 for a box of 100, depending on the vendor. The cost of vials of insulin vary but typically run between $200 to $300 for a month’s supply. Generic versions of insulin can cost considerably less, so shopping around and doing some research could save money. But consult with your doctor and provide the details to ensure you are getting the right insulin. Contrast that with insulin pens, which can cost hundreds of dollars per pack. A pack of five pens can cost around $500. Assuming an adult weighing 80 kilograms (176 pounds) requires a small amount of 0.3 units per kilogram, or 24 units per day, that pack would last about two months.
9. Reusability
Because their selling point is convenience and ease of use, many popular insulin pens come preloaded with insulin and are thrown away after they are depleted. (The separate single-use needles used on these pens should be treated as medical waste and disposed of accordingly.) But there are also insulin pen models on the market that allow users to use insulin-loaded cartridges.
[in-text-ad-2]
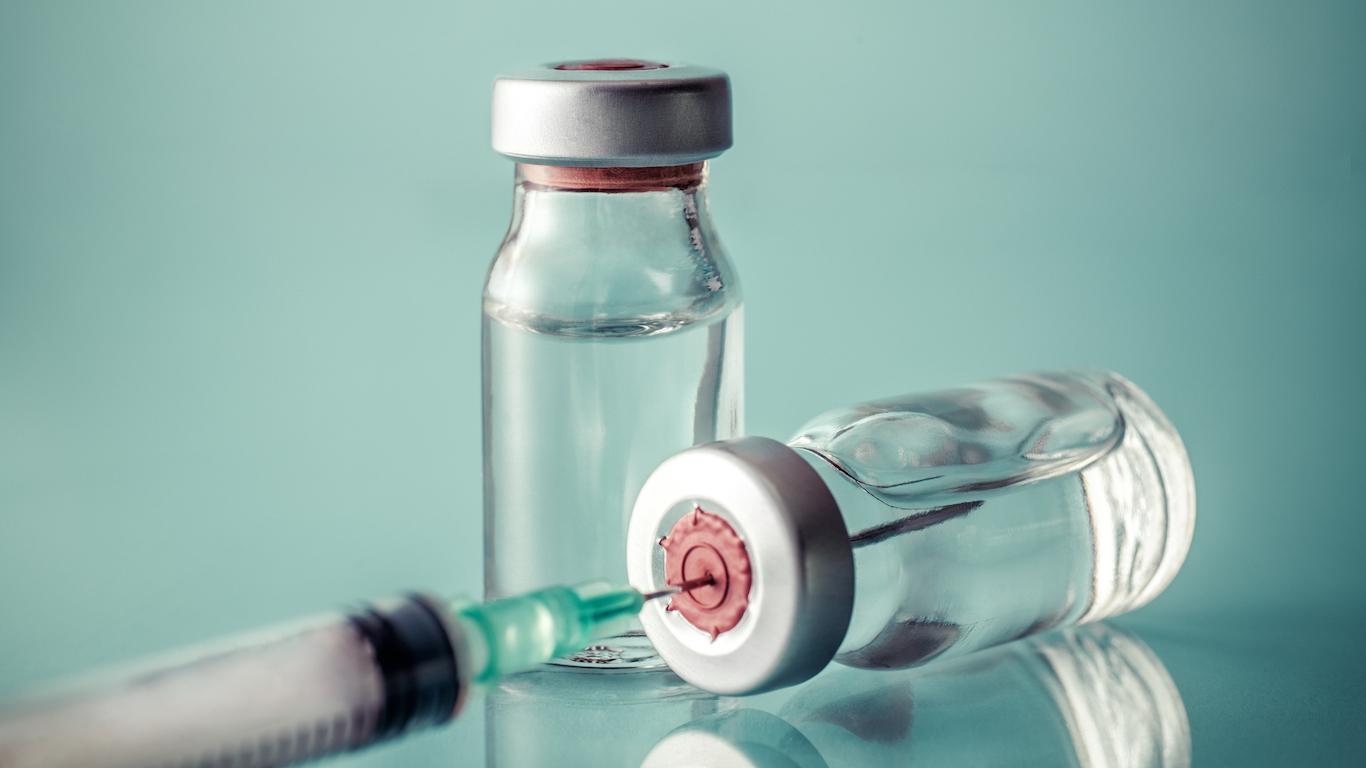
10. Types of insulin
Diabetes treatment is complicated by the fact that it depends on an individual’s metabolism and diet, level of insulin resistance, and the amount of time a patient has had the disease. This affects dosage sizes and the frequency of insulin injections. On top of that, there are five different kinds of insulin: rapid-acting, taken before or after meals; short-acting, taken about 30 minutes before a meal; intermediate-acting, which controls sugar levels for about 12 hours at a time; long-acting, which can last for 20 hours to 26 hours; and pre-mixed, a combination of intermediate- and short-acting insulin, typically taken twice a day 10 minutes to 30 minutes before eating and lasts 10 hours to 16 hours.
Sponsored: Attention Savvy Investors: Speak to 3 Financial Experts – FREE
Ever wanted an extra set of eyes on an investment you’re considering? Now you can speak with up to 3 financial experts in your area for FREE. By simply
clicking here you can begin to match with financial professionals who can help guide you through the financial decisions you’re making. And the best part? The first conversation with them is free.
Click here to match with up to 3 financial pros who would be excited to help you make financial decisions.
 24/7 Wall St.
24/7 Wall St.