Most chronic conditions have symptoms. They may be mild and vague but they often appear. Sometimes, however, a disease is silent and shows no signs until it’s reached an advanced stage. This is why health organizations recommend screening tests — to look for an illness, even before any signs appear so it’s caught early enough to treat successfully.
Men have a shorter life expectancy than women, and in addition to the hormonal and genetic differences that might help explain this variation, another possible explanation is cultural conditioning. Men are more likely to simply “man up” and see a doctor only when they are pressured by a loved one or when their condition has significantly worsened.
24/7 Tempo has compiled a list of examinations men should have and when, using sources such as the Centers for Disease Control and Prevention, National Institutes of Health, and the National Cancer Institute.
While anyone can develop medical issues like cancer or heart disease, men are much more likely to face these and other life-threatening illnesses — these are 12 health problems that afflict more men than women.
Click here for the 24 medical tests every man should have and when

1. Diabetes
> When to get tested: 45 and over every 3 years
About 10.5% of the U.S. population has diabetes — that’s more than 34 million Americans, according to the American Diabetes Association. Another 7.3 million don’t know they have the condition, which if left uncontrolled can lead to blindness, kidney failure, limb amputation, and cardiovascular disease. One in three adults have prediabetes, and most are not aware or have never been told they have the condition. Men are more likely than women to develop type 2 diabetes, because they tend to accumulate fat around the liver and waist.
There are several blood sugar tests that can confirm a diabetes diagnosis. The standard test for the illness is the glycated hemoglobin (A1C) test, which measures the average blood sugar levels over a period of two to three months. Screening is recommended at three-year intervals beginning at age 45, unless a person is at higher risk for diabetes because they are overweight, have a family history of the condition, or do not exercise.
[in-text-ad]
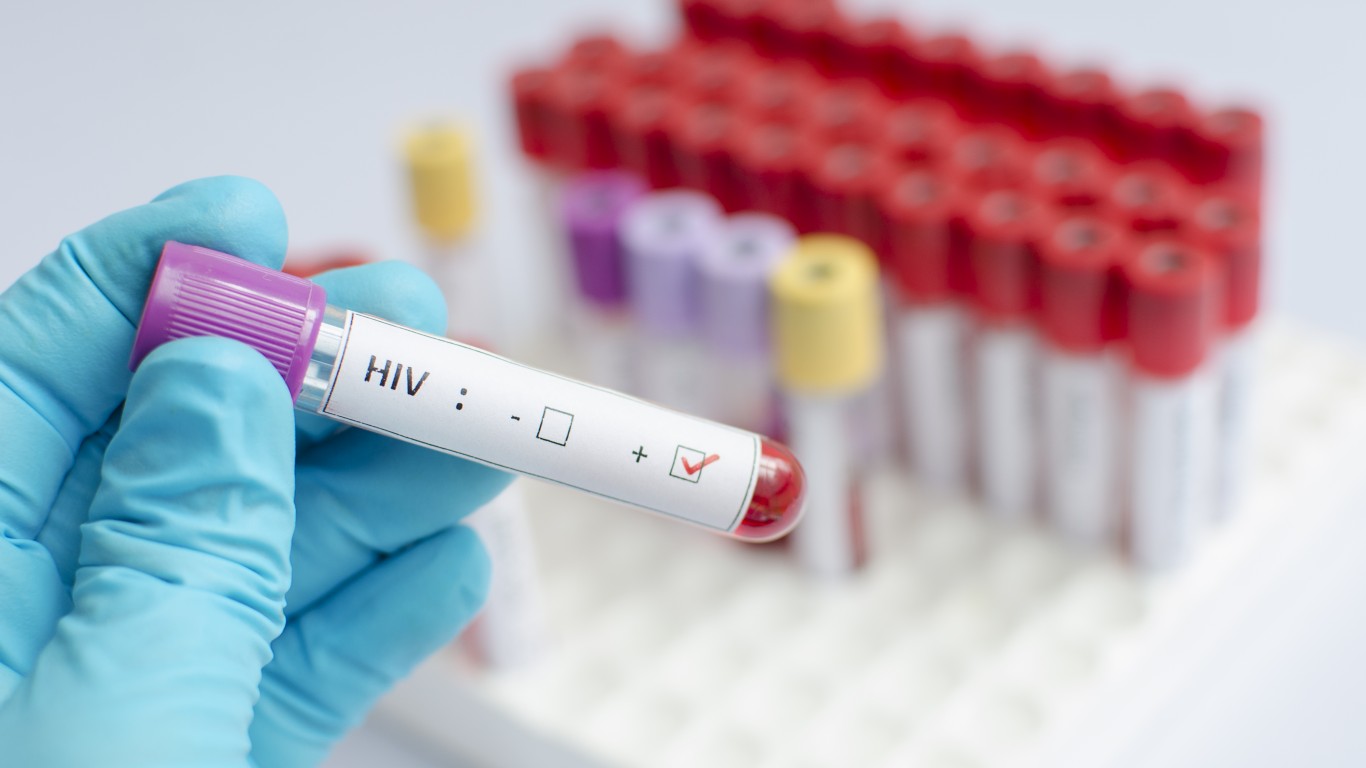
2. HIV
> When to get tested: Between 13 and 64
About 1.1 million people in the United States have HIV (the human immunodeficiency virus), but about 14% of them — more than 162,000 people — are unaware of their status, according to the CDC. Nearly 40% of new infections are transmitted by HIV-positive people who don’t know they carry the virus. HIV is usually transmitted through unprotected sex or sharing needles.
Several lab and home tests are available. The Food and Drug Administration recommends blood antibody/antigen combination tests because tests checking only for antibodies can produce false negatives. Antibodies take up to eight weeks to develop after exposure to the virus. The CDC recommends people between 13 and 64 to get tested at least once in their lifetime for HIV. Those at higher risk, like people who engage in unroptected sex or share needles, need to be tested often. The CDC also notes that sexually active gay and bisexual men, should get tested every three to six months.
3. Other STDs and STIs
> When to get tested: Once a year
The numbers of sexually transmitted diseases in the United States increased for a fifth year in a row in 2018, reaching all-time highs, according to the CDC. Half of all new sexually transmitted infections (STIs) that occur every year nationwide are among young people aged 15-24.
Two of the most common STDs in both men and women are chlamydia and gonorrhea. The rate of reported chlamydia cases among men has increased every year between 2000 and 2018, except between 2012 and 2013 when the rate was stable. There are several tests used to detect infectious diseases, including using a blood or a urine sample or a swab from the genitals.
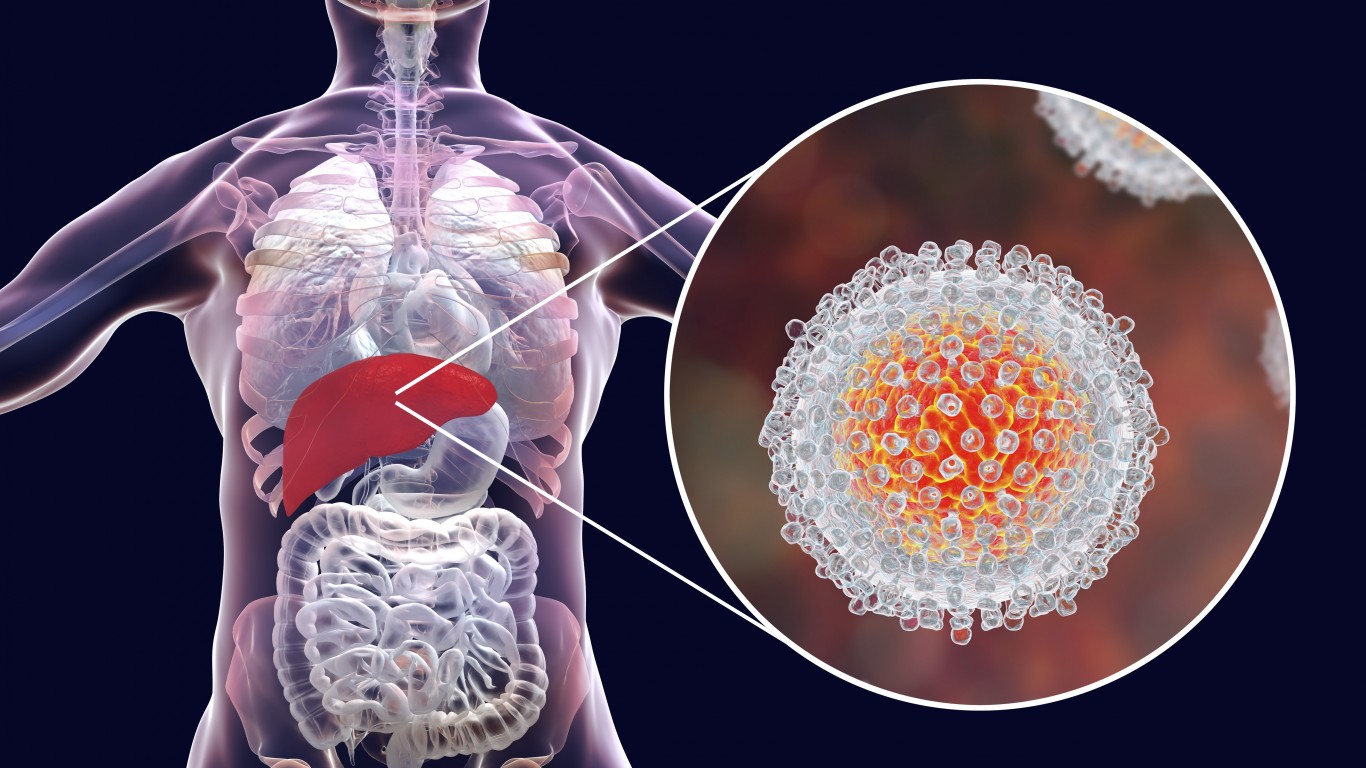
4. Hepatitis C
> When to get tested: People born between 1945 and 1965
Men are slightly more likely than women to have hepatitis C, a viral infection that damages the liver, or develop severe side effects as a result of the disease. Hepatitis C spreads through the blood of an infected person. People sharing needles or getting tattoos or piercing with unsanitary equipment are at higher risk. More than 3 million people in the country have hepatitis C, but most don’t have any symptoms and don’t know they are infected. About 17,000 new cases are diagnosed every year. If left untreated, the infection can lead to cirrhosis, liver cancer, or death.
The CDC recommends hepatitis C screening, which consists of a simple blood test, at least once for all adults as well as for all people who have HIV or have undergone certain medical procedures. Everyone born between 1945 and 1965 — the baby boomers — should get tested for hepatitis C. More than 75% of Americans living with the condition are baby boomers, according to the American Liver Foundation.
[in-text-ad-2]
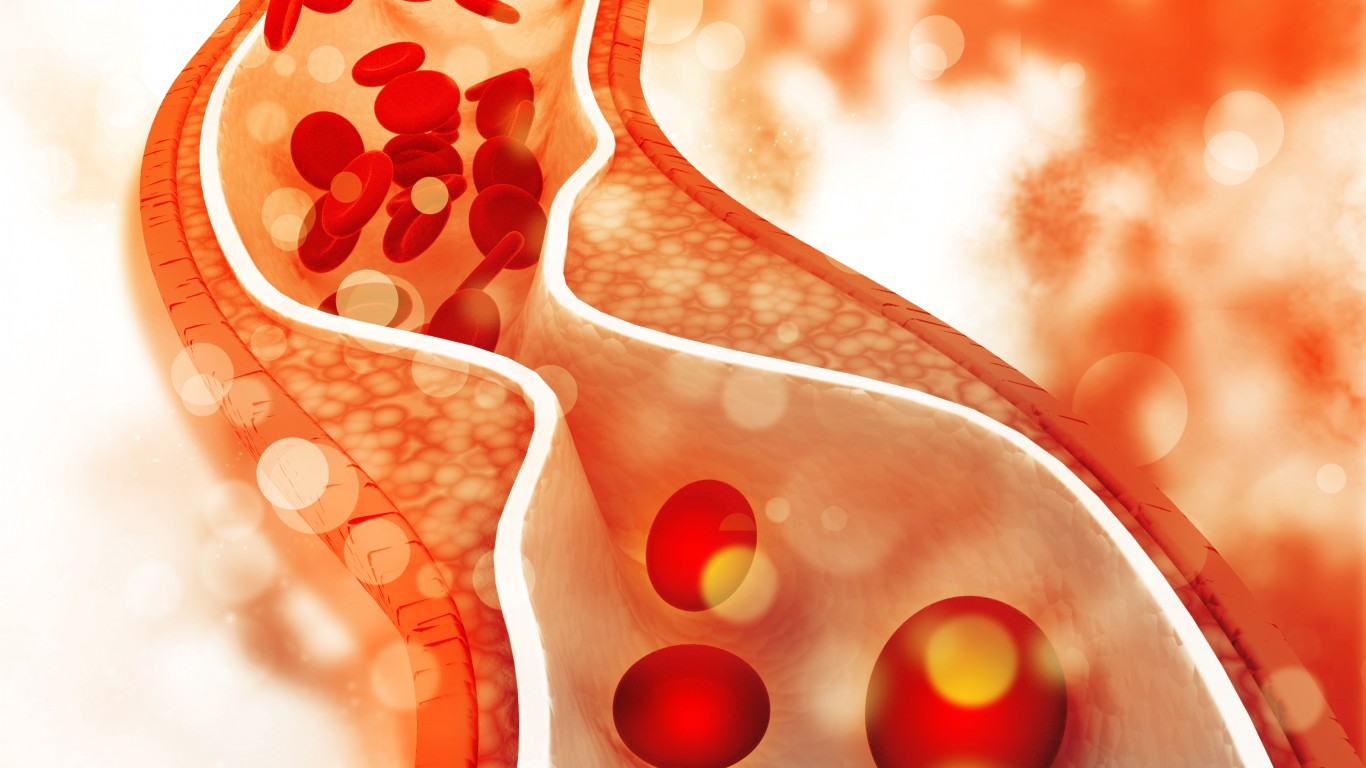
5. Cholesterol
> When to get tested: Every 4 to 6 years after 20
There are two main types of cholesterol — the good, or HDL cholesterol, and the bad, or LDL cholesterol. A simple blood test can measure the level of each type of the fat-like substance found in a person’s blood and every cell of the body. High LDL levels are dangerous as they may lead to plaque build-up in the arteries, which can block blood flow, increasing the risk of a heart attack and stroke. High cholesterol levels usually show no symptoms.
The American Heart Association recommends that everyone over the age of 20 should have their cholesterol checked every four to six years. More frequent testing may be needed for people who are at higher risk for developing heart disease, including those who are overweight, have diabetes, smoke, and are physically inactive.

6. Body fat percentage
> When to get tested: Every few months
Body mass index (BMI), which is a measure of body fat based on height and weight, is the standard doctors use to diagnose obesity or if a person is overweight. BMI, however, has limitations. It does not distinguish fat from muscle and does not take into account how much of the weight is actually fat. Too much body fat can increase the risk of health issues such as high cholesterol, heart disease, and even depression. Excessive abdominal fat may increase the risk of type 2 Diabetes, hypertension, and coronary artery disease.
Men store more fat around the stomach, which is more dangerous than storing it on the hips and thighs as women generally do. Visceral fat increases the risk of cardiovascular disease, insulin resistance, high blood pressure, diabetes, colon cancer, and sleep apnea.
A more comprehensive body fat calculator takes into account age, gender, weight, height, as well as skinfold measurements of the thighs, triceps, and suprailium (above the upper bone of the hip). The healthy range for men is between 2% and 24%, depending on age and level of physical activity.
[in-text-ad]
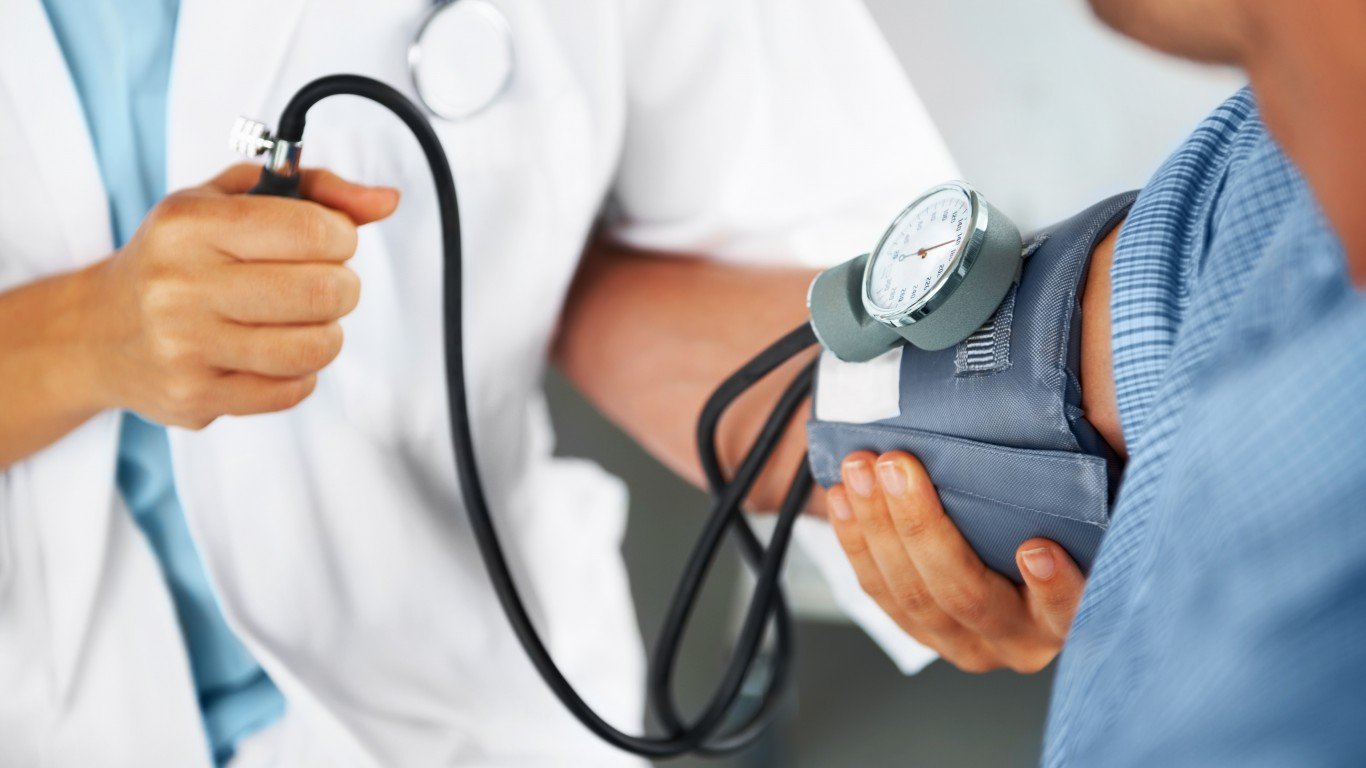
7. Blood pressure
> When to get tested: At least every two years after 18
Health organizations released new guidelines in 2017 about normal blood pressure, lowering the hypertension diagnosis level to 130/80 from the previous threshold of 150/80 for older than 65 and 140/90 for younger than 65. Following the change, between 70% and 79% of men were now classified as having hypertension. High blood pressure is often called “the silent killer” because symptoms don’t show up until vital organs are already damaged.
When left untreated, the condition can damage the heart and lead to heart disease, stroke, and kidney disease. In the decade between 2005 and 2015, the death rate from hypertension-related causes has increased by 11% in the U.S., according to the American Heart Association.
People can check their blood pressure regularly with home blood pressure monitors. Otherwise, the recommendation is for people with no history of hypertension to get their blood pressure checked at least every two years or every year if their blood pressure is borderline high.
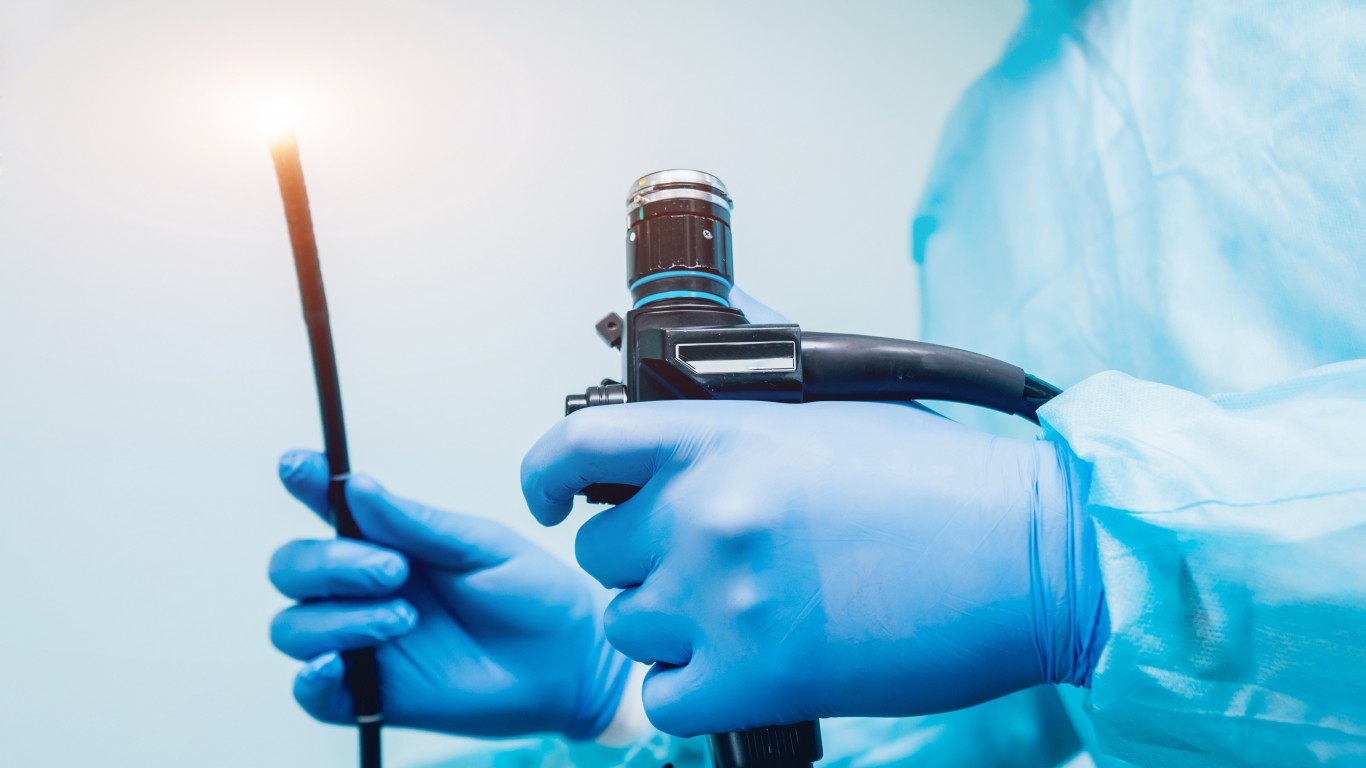
8. Colonoscopy
> When to get tested: At least every 10 years after 50
Men and women between the ages of 50 and 75 should get a colonoscopy, which is used to screen for colorectal cancer, at least every 10 years, according to the National Institutes of Health. The American Cancer Society recommends that people start regular screening at age 45. Men are at a slightly higher risk than women of developing colorectal cancer.
Colorectal cancer is the third most common cancer diagnosis among both men and women (excluding skin cancer) as well as the third leading cancer-related cause of death in the U.S. Lifestyle factors that increase the risk of developing colorectal cancer include being overweight or obese, being physically inactive, eating a diet high in red and processed meats, smoking, and excessive drinking.
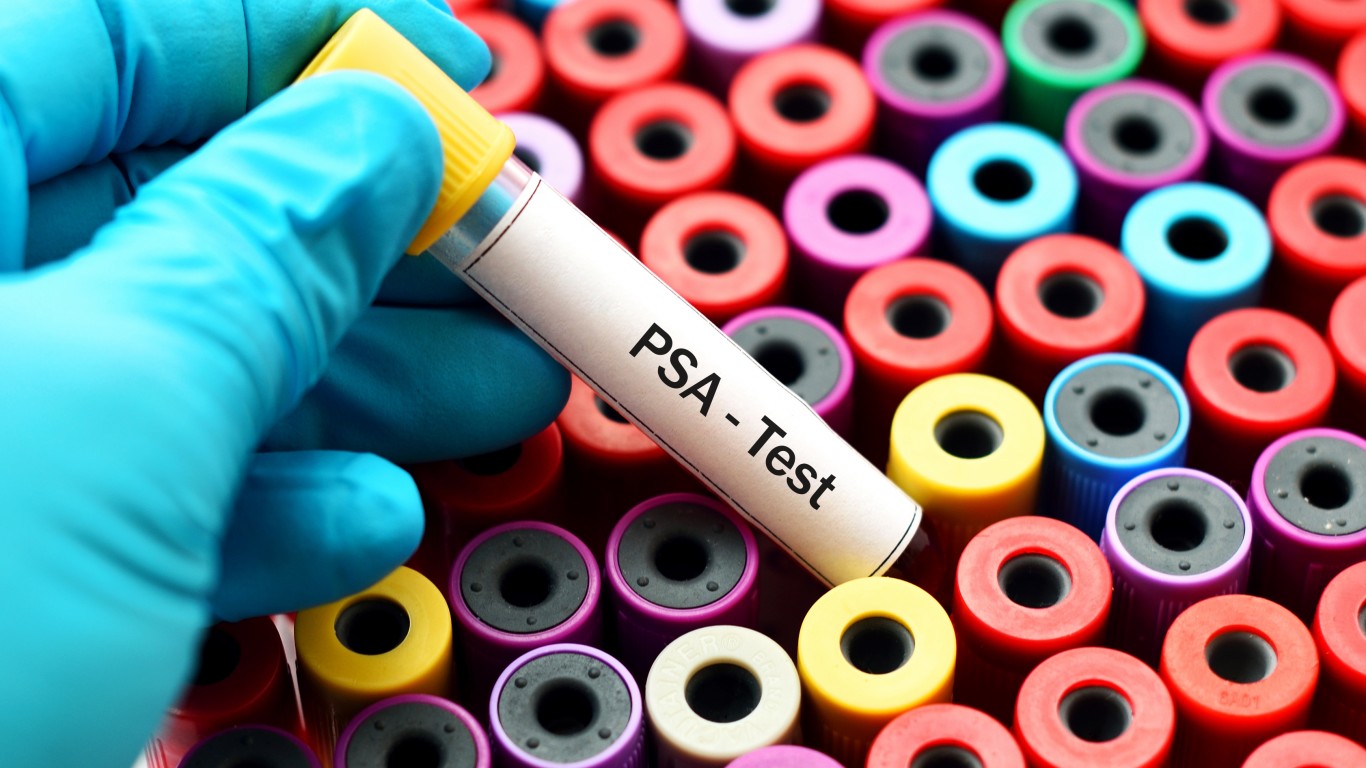
9. Prostate-specific antigen (PSA) blood test
> When to get tested: Every year after 50
The National Institutes of Health recommends that men over the age of 50 begin screening for prostate cancer, the second most common cancer among men in the country after skin cancer. The recommendation for African American men and those with a family history of the disease is to start at 45.
The routine screening test is called the prostate-specific antigen (PSA) test. PSA is a protein produced by both cancerous and noncancerous tissue in the prostate. High PSA level may indicate cancer, but it can also mean enlarged prostate. There is still a debate about the harm versus benefits of the PSA tests as they may detect minor cancers and result in unnecessary treatments.
About 12% of men will be diagnosed with prostate cancer in their life, according to the National Cancer Institute. Prostate cancer is estimated to make up about 10.6% of all new cancer cases and 5.5% of all cancer-related deaths in 2020.
[in-text-ad-2]

10. Depression
> When to get tested: If symptoms last more than 2 weeks
While women are more likely to be diagnosed with clinical depression, men are about four times more likely to commit suicide than women, according to the CDC. About 9% of American men experience feelings of depression or anxiety every day, according to a National Health Interview Survey published in 2015. Nearly a third of men in the country have suffered from depression at some point in their life, according to a 2013 study in JAMA Psychiatry. Suicide was the second leading cause of death among people of both sexes between 10 and 34 years old in 2017.
Depression screening typically involves questionnaires, such as the Patient Health Questionnaire, the Hospital Anxiety and Depression Scale for medical patients, the Geriatric Depression Scale in older adults. The new guidelines by the U.S. Preventive Services Task Force recommend that all people age 18 and older be screened for depression.
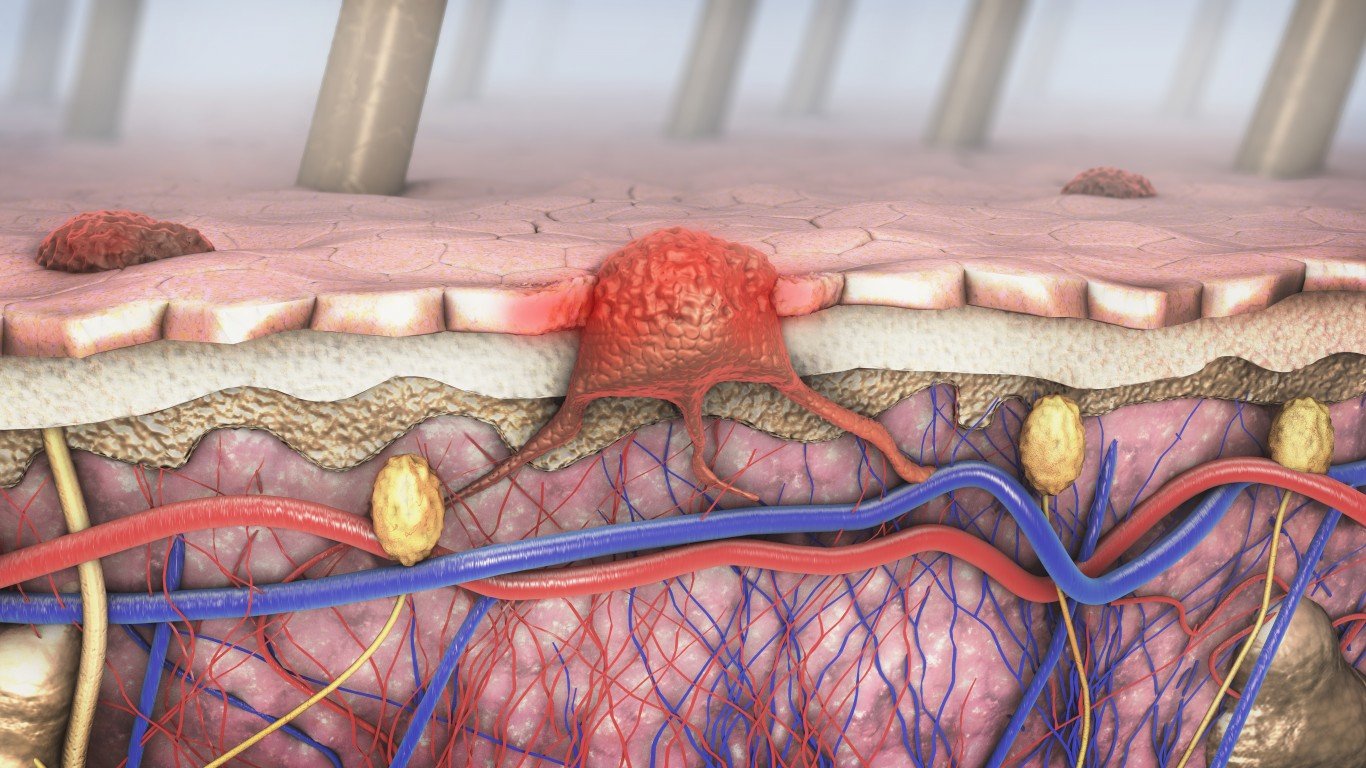
11. Melanoma
> When to get tested: Every year
Melanoma is the most serious type of skin cancer and can appear anywhere on the body, including in the eyes and inside the nose or throat. Men have a higher risk of developing this type of cancer than women, and they are more likely to die of melanoma than women. This may be due to men knowing less about skin cancer and its risk factors, according to a survey conducted by the American Academy of Dermatology in 2016.
The American Academy of Dermatology recommends that people get a full skin exam once a year in order to check for signs of skin cancer. The exams, which should be conducted by a dermatologist, look for unusual or suspicious moles or markings on the skin. Nearly 78,000 new cases of melanoma were diagnosed in the U.S. every year between 2012 and 2016, according to the CDC. About 46,000 of each year’s new melanoma cases were in men.
[in-text-ad]
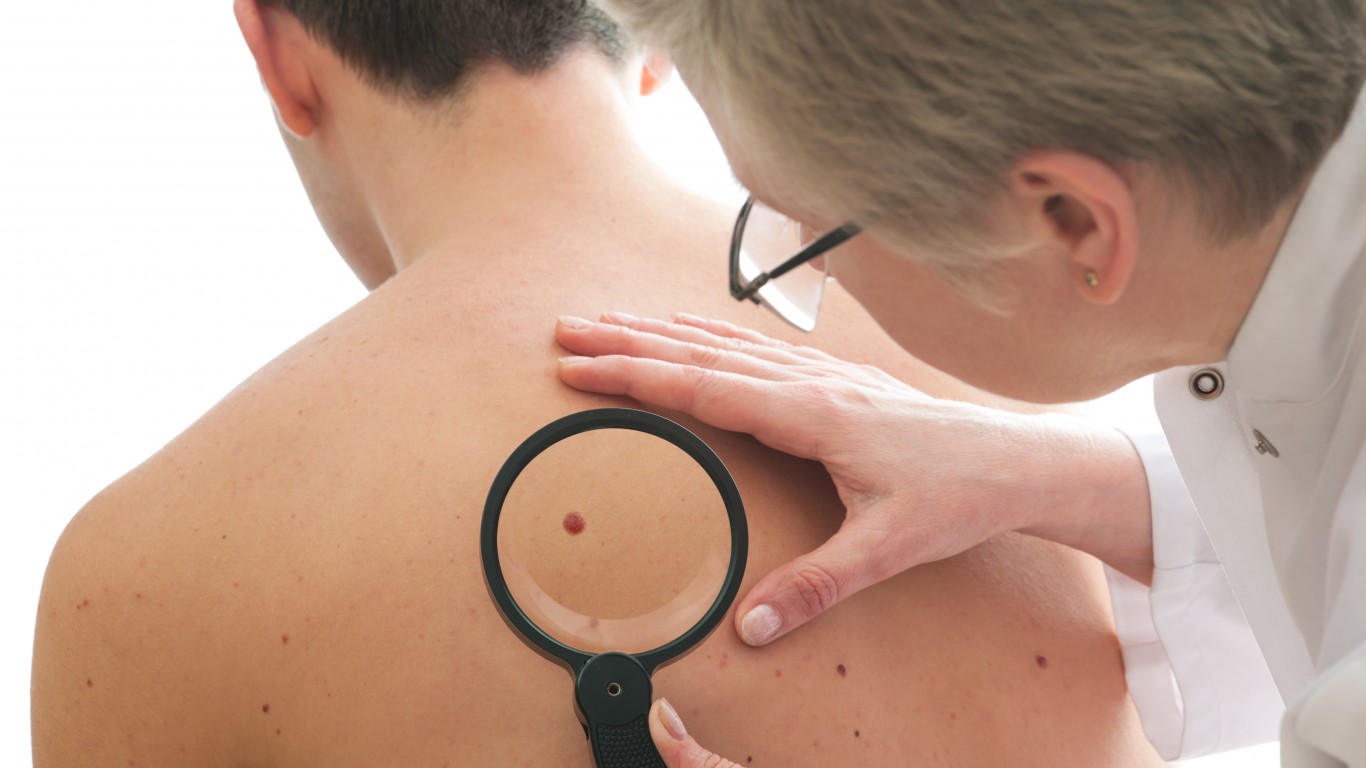
12. Other skin cancers
> When to get tested: Once a year
Skin cancer is the most common type of cancer in the U.S., according to the American Cancer Society. More than two people die of skin cancer in the country every hour, according to the Skin Cancer Foundation. Non-melanoma skin cancer is also more common in men than in women.
Annual full-body exams by a dermatologist are recommended for people with a history of melanoma or skin lesions, those who have family history of skin cancer, and those who have a lot of moles or a history of atypical moles, have had an organ transplant, or have a history of significant sun exposure. Other skin cancer risk factors include fair skin, sunburns, exposure to radiation, and living in high-altitude climates where the sunlight is stronger.
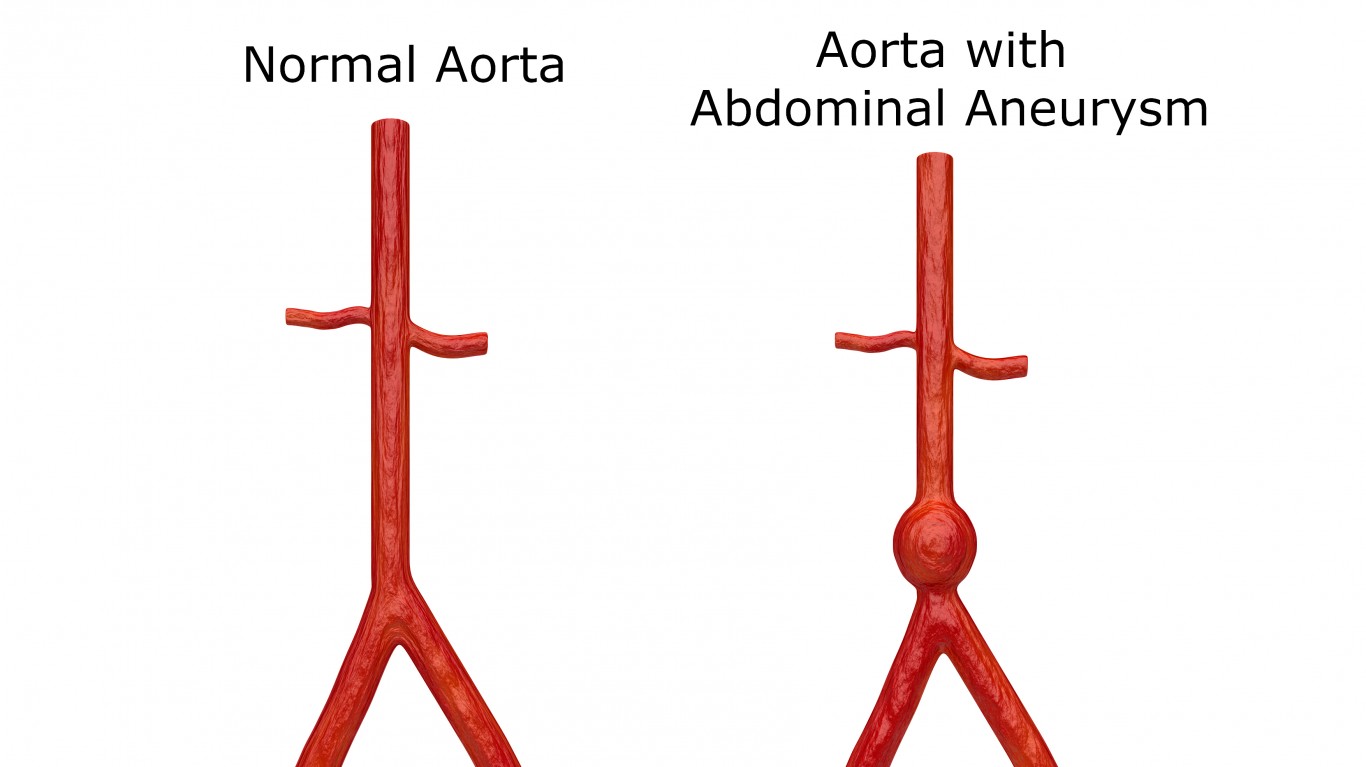
13. Abdominal aortic aneurysm (AAA)
> When to get tested: Between 65 and 75
Abdominal aortic aneurysm is an enlargement of the main blood vessel that delivers blood to the body. The aorta runs from the heart through the center of the chest and abdomen. An aneurysm can be fatal if it bursts. Symptoms of an abdominal aortic aneurysm include constant stomach pain, back pain, and a pulse near the abdomen.
Men develop abdominal aortic aneurysms much more often than women do. The disease has a 4:1 male to female predominance. The U.S. Preventive Services Task Force recommends a screening test, which uses high-frequency sound waves, for men between 65 to 75 who have a history of smoking.
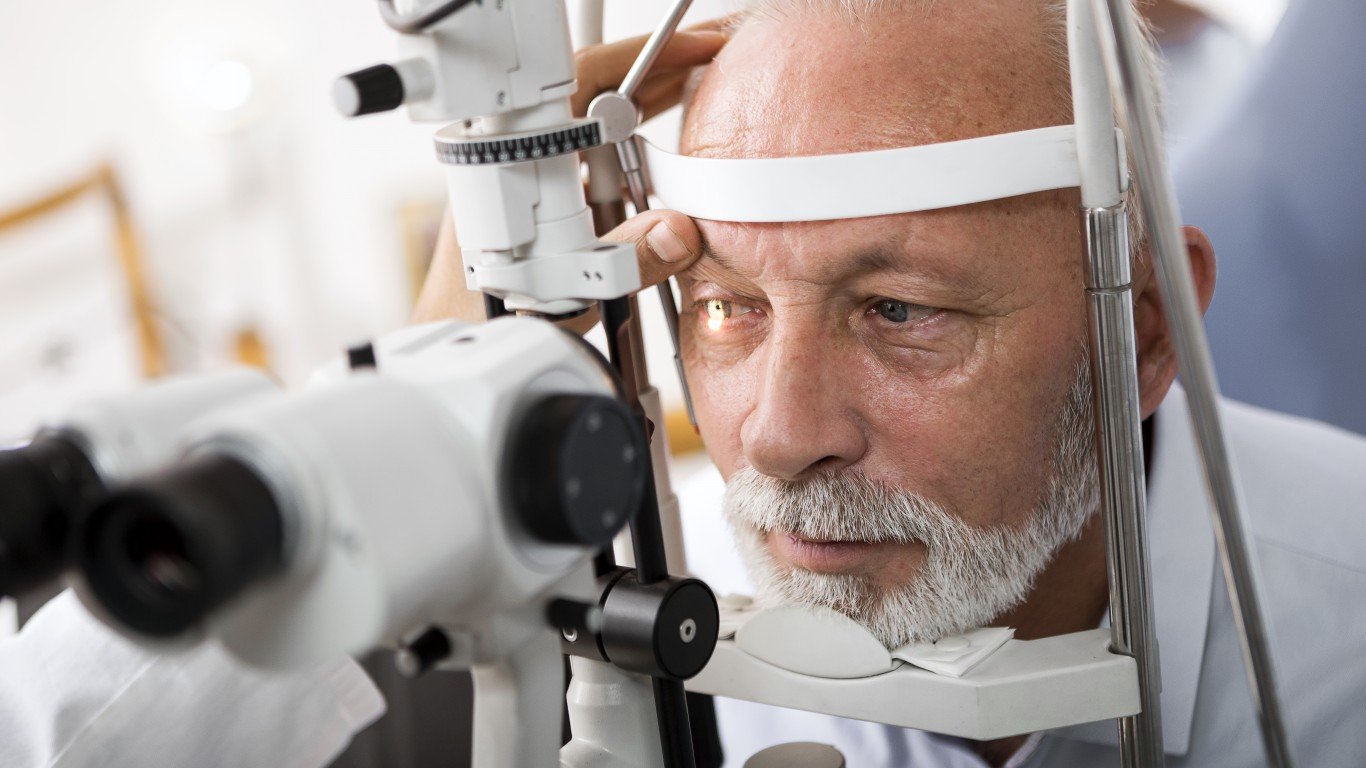
14. Glaucoma
> When to get tested: After 40
There are several types of glaucoma, a condition that affects the nerve connecting the eye to the brain. The most common type of glaucoma is an open-angle glaucoma, which often has no symptoms other than gradual vision loss. Glaucoma, which has no cure, is a leading cause of irreversible blindness in the U.S. More than 3 million Americans are living with glaucoma, but half of them don’t even know it, according to the Glaucoma Research Foundation.
African American men and all men who have a family history of glaucoma are at higher risk of the disease. The American Academy of Ophthalmology recommends an eye disease screening for everyone over the age of 40. People at higher risk — such as diabetics, those with high blood pressure, and people with family history of glaucoma — should start testing earlier.
[in-text-ad-2]
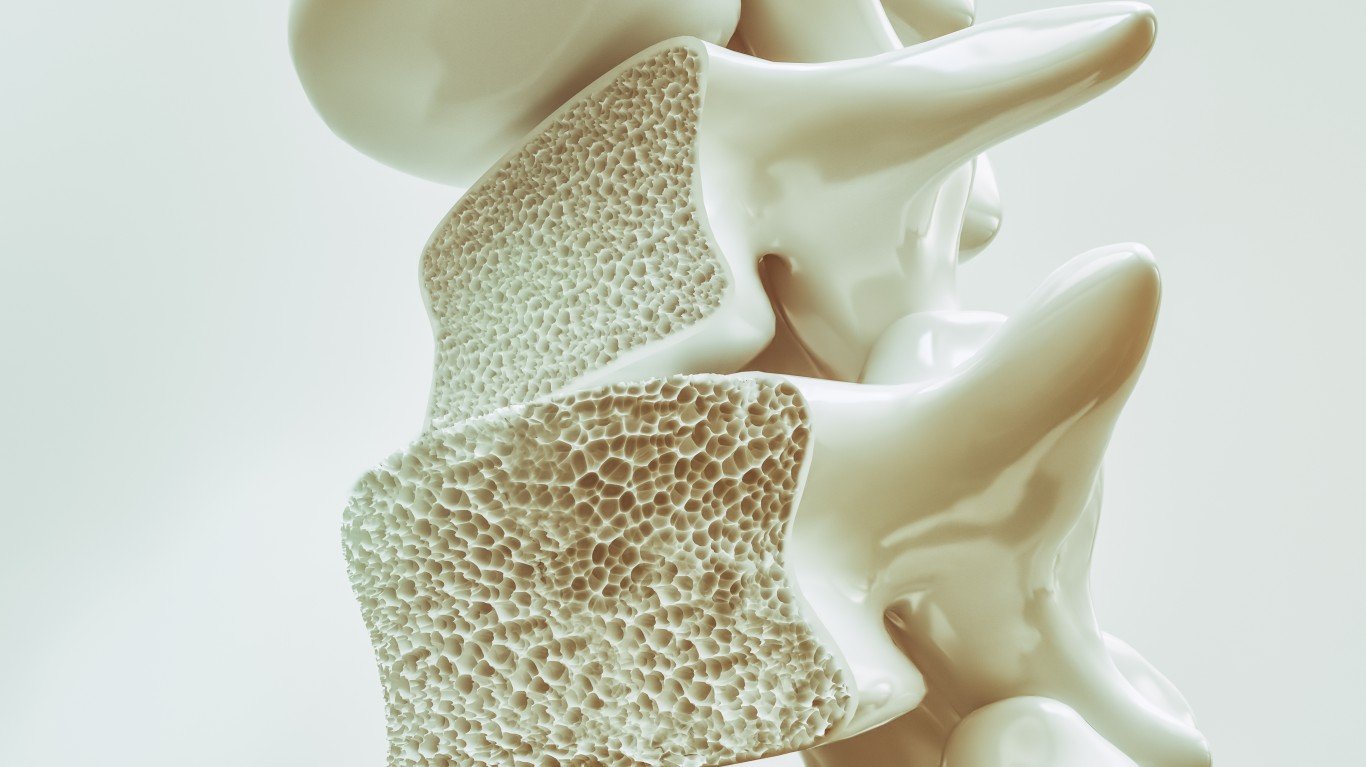
15. Osteoporosis
> When to get tested: After 70
Osteoporosis is a condition that causes the bones to become weak and brittle, increasing the risk of major bone fractures even after bending. Most people don’t even know they have osteoporosis until a fracture occurs because the disease progresses slowly without symptoms. Compared to men, women tend to develop osteoporosis earlier in life, and it progresses faster in women because they have less bone mass. Still, osteoporosis in men has been recognized as a serious public health issue.
The National Osteoporosis Foundation recommends that all men over the age of 70 or men over the age of 50 who have risk factors get a bone density test. Risk factors include certain medications, low testosterone levels, thyroid problems, excessive drinking, smoking, having stomach or intestine diseases, and prolonged bed rest.
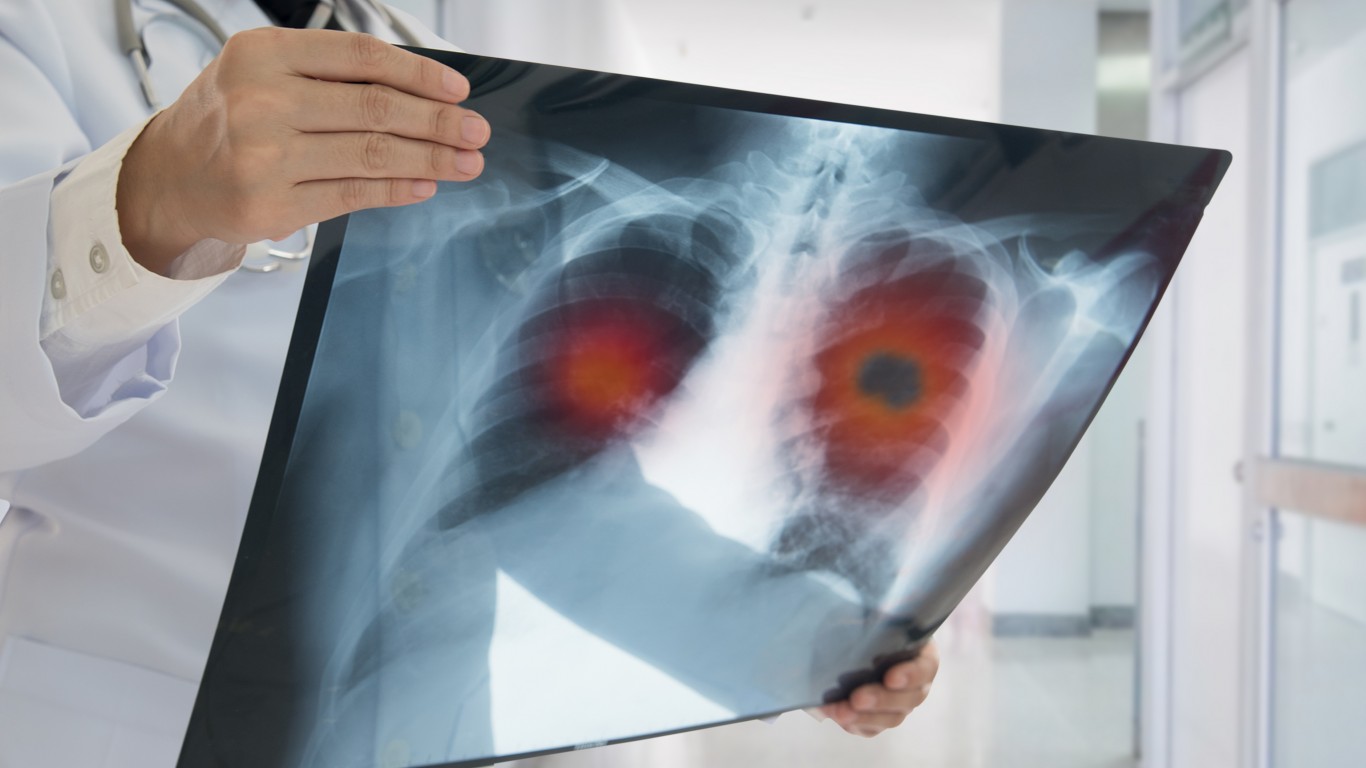
16. Lung cancer
> When to get tested: Adults ages 55 to 80 years
Lung cancer is the deadliest cancer among both men and women in the United States. It’s difficult to detect in early stages. Partially as a result, more than half of the patients die within a year of being diagnosed. More men than women are diagnosed with lung cancer each year, and men are slightly more likely to die from the disease. The age-adjusted death rate is higher for men than for women, at 46.7 lung cancer deaths per 100,000 men and 31.9 per 100,000 women, respectively.
A low-dose computed tomography (a low-dose CT scan, or LDCT) is the only lung cancer screening test recommended by the CDC. Asymptomatic people with a history of smoking and people who are between 55 and 80 should be screened every year, according to the U.S. Preventive Services Task Force.
[in-text-ad]
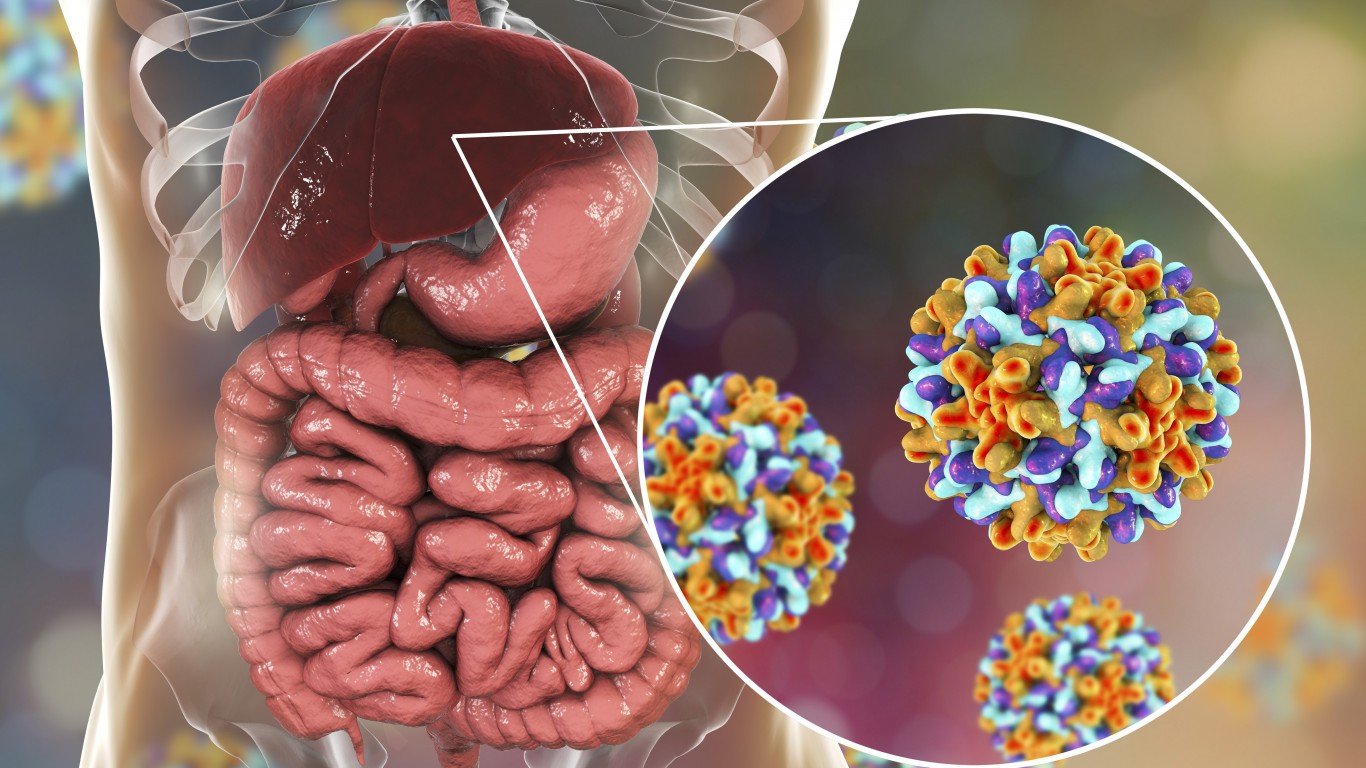
17. Hepatitis B
> When to get tested: Anytime unless vaccinated
Hepatitis B, a viral infection that attacks the liver, affects men more severely than women. Men are more than twice as likely to develop liver disease such as cirrhosis or liver cancer as a result of having hepatitis B infection. It’s yet unclear why this is the case. A vaccine can prevent hepatitis B, but it’s recommended, not required.
About 80,000 Americans become infected every year with hepatitis B. Screening with a basic blood test is recommended for adolescents and adults at high risk of chronic infection. People at higher risk include those who share needles, gay men, medical workers exposed to human blood, and those who have traveled to regions with high hepatitis B infections.
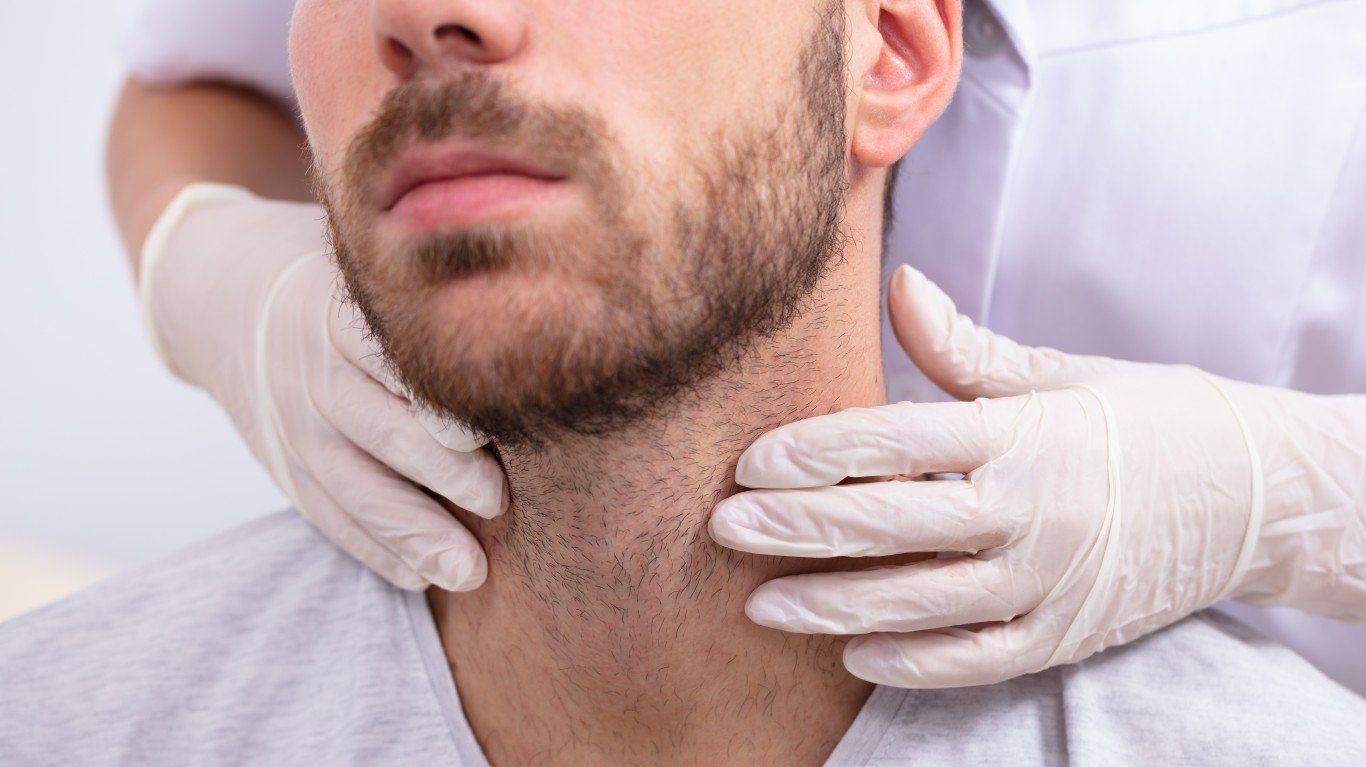
18. Thyroid
> When to get tested: After 60
Thyroid problems, which are screened for with a blood test, are caused by either too many or too few thyroid hormones produced by the butterfly-shaped gland at the base of the neck. The thyroid plays a role in many vital body functions such as heart rate and metabolism, and it helps regulate mood, muscle strength, body weight, energy levels, and cholesterol, to name a few.
Though more women than men have thyroid disease, including thyroid cancer, it is fast-rising cancer in men, and they usually have a worse prognosis, according to the American Thyroid Association. About 12,000 men (and 35,000 women) get thyroid cancer a year, and more than 900 men (and 1,100 women) die from the disease every year in the United States.

19. Vitamin D
> When to get tested: Only in individuals at risk for deficiency
Vitamin D, which is called the “sunshine vitamin” because the body produces it when the sun’s ultraviolet rays come in contact with the skin, helps the body absorb calcium and sustain strong bones. Vitamin D deficiency has been linked to several cancers, heart disease, depression, muscle pain, diabetes, and infections. People with dark skin are at higher risk of vitamin D deficiency as the darker the skin, the more sun it needs to absorb to produce enough vitamin D.
Vitamin D deficiency is common in older men and is prevalent in obese, sedentary men living at higher latitudes. Vitamin D levels are checked with a simple blood test that can be part of a routine medical exam.
[in-text-ad-2]
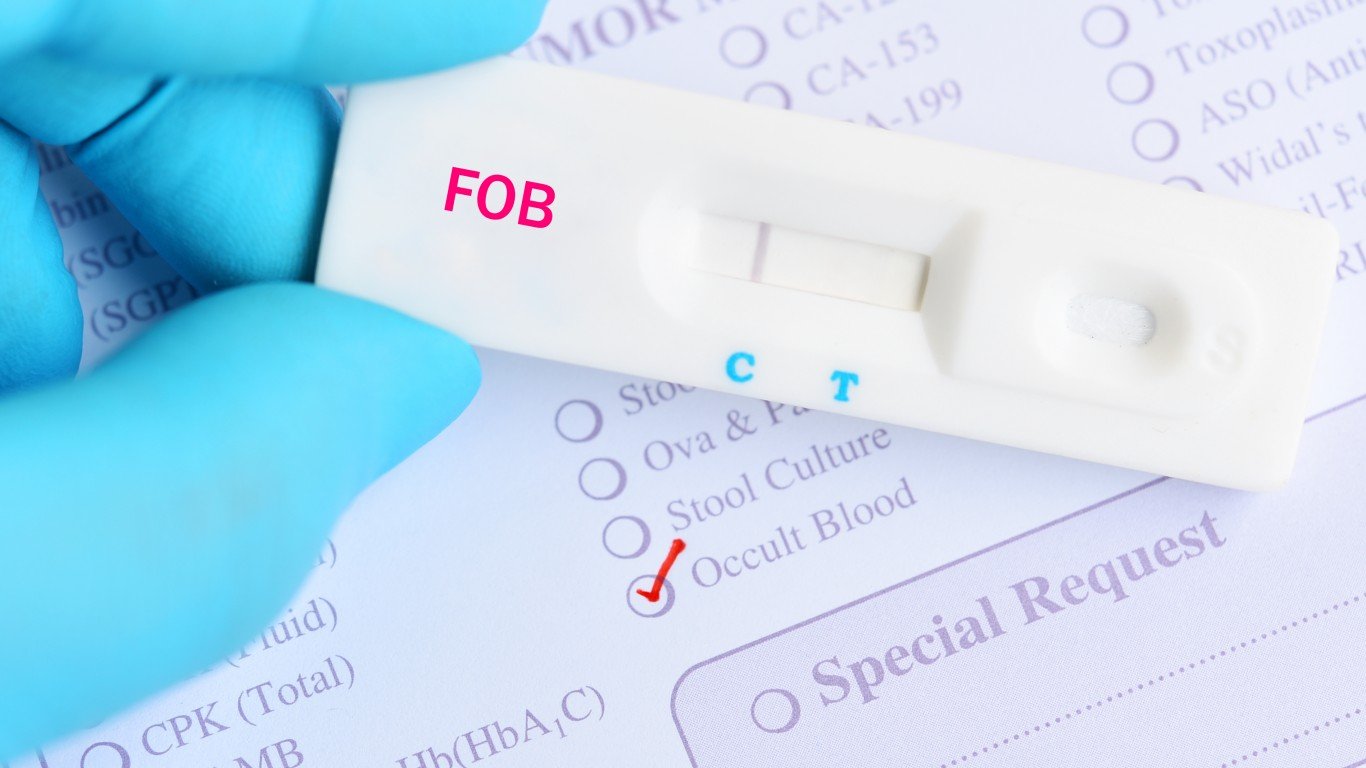
20. Fecal occult blood test (FOBT)
> When to get tested: After 50
Fecal occult blood test, which is sometimes used to detect colorectal cancer at early stages, is a lab test used to check stool samples for hidden blood. The test may also indicate ulcers or inflammatory bowel disease.
The National Cancer Institute recommends that people get regular screenings for colorectal cancer starting at age 50. If the test is positive, a doctor may recommend a colonoscopy. A FOBT test is recommended every year, while a stool DNA test, which checks for blood and genetic changes that may be signs of cancer, should be done every three years.

21. Audiogram
> When to get tested: Every 10 years for adults up to the age of 50
An audiogram is basically a hearing test showing how loud sounds need to be for a person to hear them. The test is used to show the type, degree, and configuration of hearing loss. Men are twice as likely as women to experience hearing loss among adults aged 20-69, but they are less likely than women to seek help, according to the National Institute on Deafness and other Communication Disorders. The most hearing loss occurs in adults between 60 and 69 years of age.
People are advised to get their hearing tests after the age of 21 to determine a baseline. This helps determine how exactly one’s hearing has changed over time. If a person has no hearing loss, he or she should have an audiogram every decade until age 50 and every three years after that.
[in-text-ad]

22. Metabolic syndrome
> When to get tested: After 50
Metabolic syndrome, which is a combination of high blood pressure, high blood sugar, excess belly fat, and high cholesterol levels, affects about 23% of U.S. adults, according to the American Heart Association. People with metabolic syndrome are at higher risk of developing cardiovascular disease, diabetes, and stroke. Some research has shown that men and elderly women are more prone to getting metabolic syndrome.
Metabolic syndrome is diagnosed if a person has three or more traits that describe the condition, including a waistline of more than 40 inches for men, high LDL “bad” cholesterol, high blood pressure, elevated fasting blood sugar, and higher triglyceride levels.
23. Bladder cancer
> When to get tested: Age 50, if you have a history of smoking
Bladder cancer occurs in men a lot more frequently than in women. The American Cancer Society estimates there will be just over 62,000 new cases in men and 19,300 new cases in women in 2020. This type of cancer is the fourth most common cancer in men. Age is a major risk factor for bladder cancer — nine in 10 people with the disease are older than 55.
Screening for bladder cancer has been called by the Canadian Urological Association “the best opportunity to reduce mortality.” There are several ways to check for bladder cancer: a test to check for blood in the urine, a test that checks for cancer cells in the urine, and a few other tests that detect substances commonly found in cancer cells.

24. Testicular exam
> When to get tested: Every year after 20
Testicular cancer is rare, making up just 1% of all cancers in men. Among men ages of 15 and 35, however, it’s the most common form of cancer, according to the Testicular Cancer Society. The diseases can almost always be cured if caught early.
According to the American Cancer Society, most doctors recommend that men be screened for the condition as part of their regular annual physical. Self-exams are recommended at least once per month.
Take This Retirement Quiz To Get Matched With A Financial Advisor (Sponsored)
Take the quiz below to get matched with a financial advisor today.
Each advisor has been vetted by SmartAsset and is held to a fiduciary standard to act in your best interests.
Here’s how it works:
1. Answer SmartAsset advisor match quiz
2. Review your pre-screened matches at your leisure. Check out the
advisors’ profiles.
3. Speak with advisors at no cost to you. Have an introductory call on the phone or introduction in person and choose whom to work with in the future
Take the retirement quiz right here.
Thank you for reading! Have some feedback for us?
Contact the 24/7 Wall St. editorial team.
 24/7 Wall St.
24/7 Wall St. 24/7 Wall St.
24/7 Wall St.