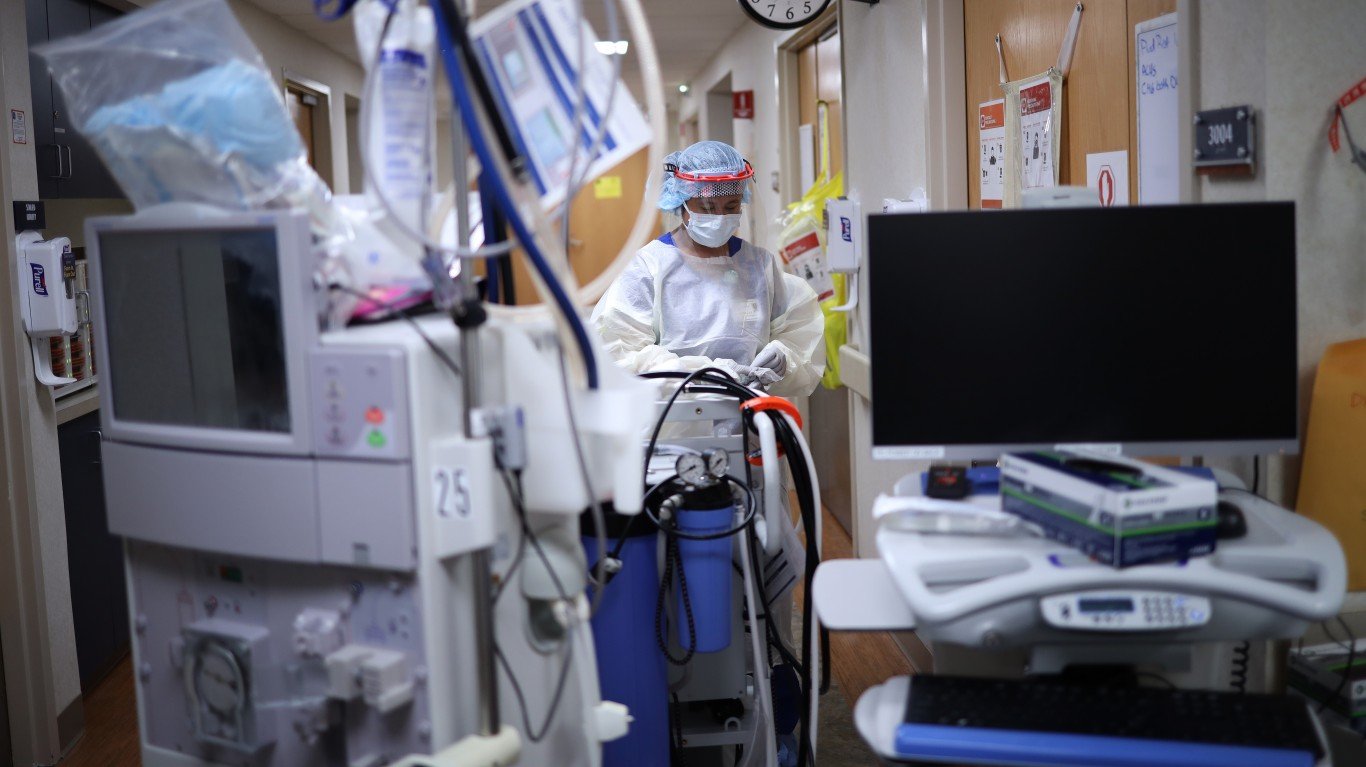
COVID-19 has overrun much of the United States. This is based on three critical measures: confirmed cases, fatal cases and the number of people in hospitals. In several cities, no intensive care unit (ICU) beds left at all. This leaves doctors with the difficult decision of what to do with severely ill patients.
Confirmed cases in the United States number 15,511,043, up by 262,461 since yesterday. The belief is strong that the increase will rise above 300,000 a day as people who traveled over Thanksgiving and contracted the disease become ill. Coronavirus deaths rose by a single-day record of 3,897 to 292,480. The Institute for Health Metrics and Evaluation (IHME) at the University of Washington’s School of Medicine forecasts that, without new mitigation rules, such deaths in the United States will reach 539,000 by April 1.
Hospitalizations for people with COVID-19 also have reached a record. The figure is over 100,000 and rising quickly.
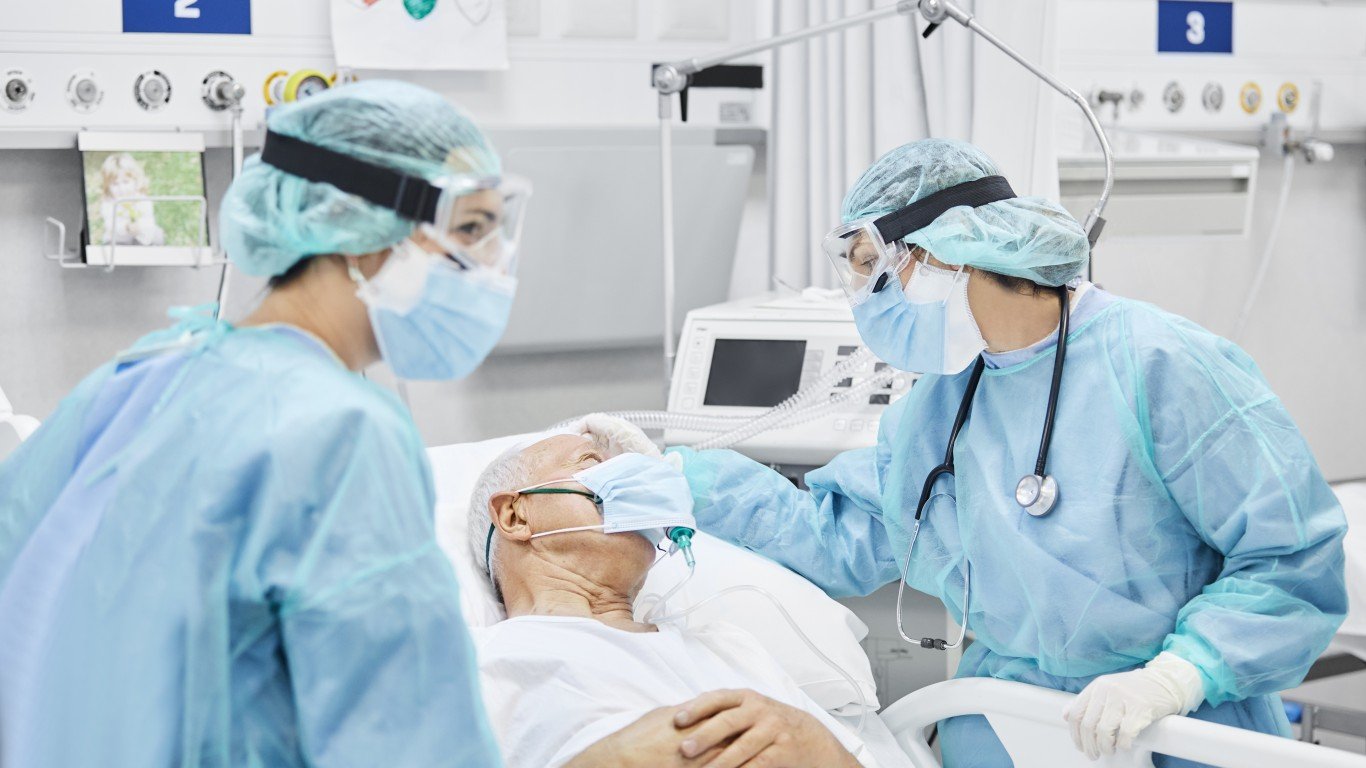
The patients who are the most severely ill require ICU beds. WebMD describes these patients as “critically ill and required treatment in an intensive care or high dependency unit.” Many such patients are put on ventilators. One study showed the average time on a ventilator is just over two weeks.
[nativounit]
The problem of a lack of ICU beds has become critical across the country. It is not isolated to one region or based on the size of a city or county. A hospital with four ICU beds in a rural area can reach maximum capacity. So can a hospital in a large city that has dozens of such beds.
One thing that is certain is that more hospitals reach ICU capacity every day. This is because daily confirmed cases are expected to rise, perhaps for months. That means the problem will worsen quickly.
Among the most horrible results of the ICU bed problem is that doctors have to triage patients based on measures such as age and severity of illness. That means some patients will not get the care they need for their health to improve.
Several organizations keep data on hospital capacity by hospital, city and county. None of these is considered definitive or 100% accurate. The standard of reporting from hospital to hospital and city to city may not be identical across the country.
One carefully followed measure, which is based on cities, is The New York Times survey of hospitals at capacity. The paper’s researchers used numbers from the Department of Health and Human Services to create their database.
24/7 Wall St. reviewed The New York Times data to screen for cities where ICU bed use is over 100%. These hospitals are not in a single area. However, there are clusters in Alabama and Pennsylvania. Note that the national average ICU occupancy is 72%.
These cities have run out of ICU beds:
| City | ICU Occupancy |
|---|---|
| Cullman, Alabama | 131% |
| Albuquerque, New Mexico | 116% |
| Ashland, Alabama | 115% |
| Hibbing, Minnesota | 114% |
| Cordele, Georgia | 109% |
| Rogers, Arkansas | 107% |
| Boaz, Alabama | 106% |
| Upland, Pennsylvania | 106% |
| Abington, Pennsylvania | 102% |
| Oxford, Mississippi | 102% |
| Foley, Alabama | 101% |
[recirclink id=824046]
[wallst_email_signup]