The pace at which COVID-19 has spread in the U.S. has slowed considerably. Deaths, at 515,138, have risen at about 2,000 a day recently. That is down from over 4,000 a day less than two months ago. However, the number remains about 20% of the world’s total. Confirmed cases, at 28,761,741, are rising at less than 100,000 most days, down from a rate of over 200,000 a day just weeks ago. The U.S. figure for confirmed cases is about 25% of the global number.
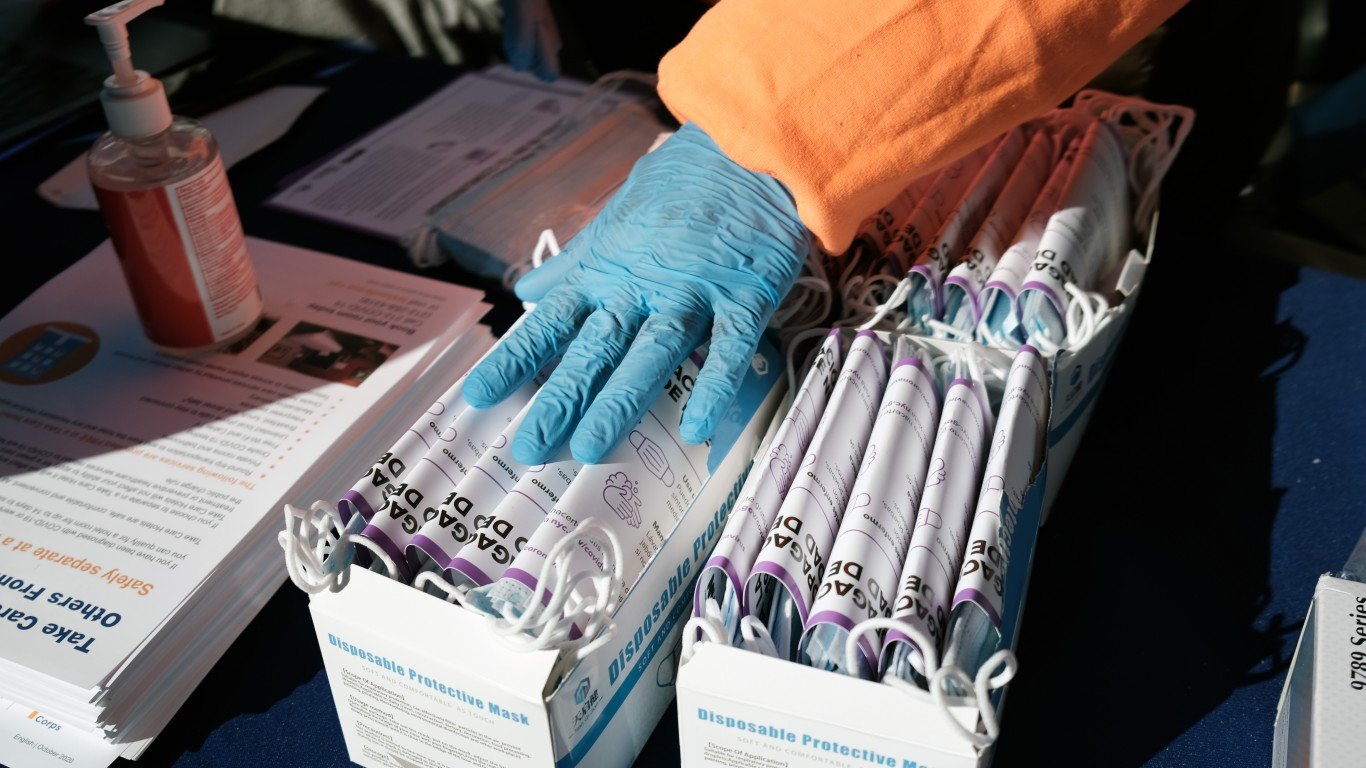
The improvements in the U.S. have been attributed to several factors. At the top of that list are vaccines, modest success with the use of masks and social distancing, and testing to locate and traces cases. Doctors have become worried that the use of tests has dropped precipitously and could help trigger another rise in the disease.
Mask wearing and social distancing have varied widely from state to state and city to city since near the start of the pandemic. Some states, particularly in the Midwest and the Plains States, did little to encourage the use of masks. At one point, the Governor of South Dakota suggested that bars that had been closed in Minnesota move to her state where there were no requirements to wear masks or curtail public gatherings. Governor Kristi Noem tweeted on December 21 “Come to South Dakota! We respect your rights. We won’t shut you down.” Fortunately, during the most recent, brutal surge, the trend toward the use of masks and social distancing has improved.
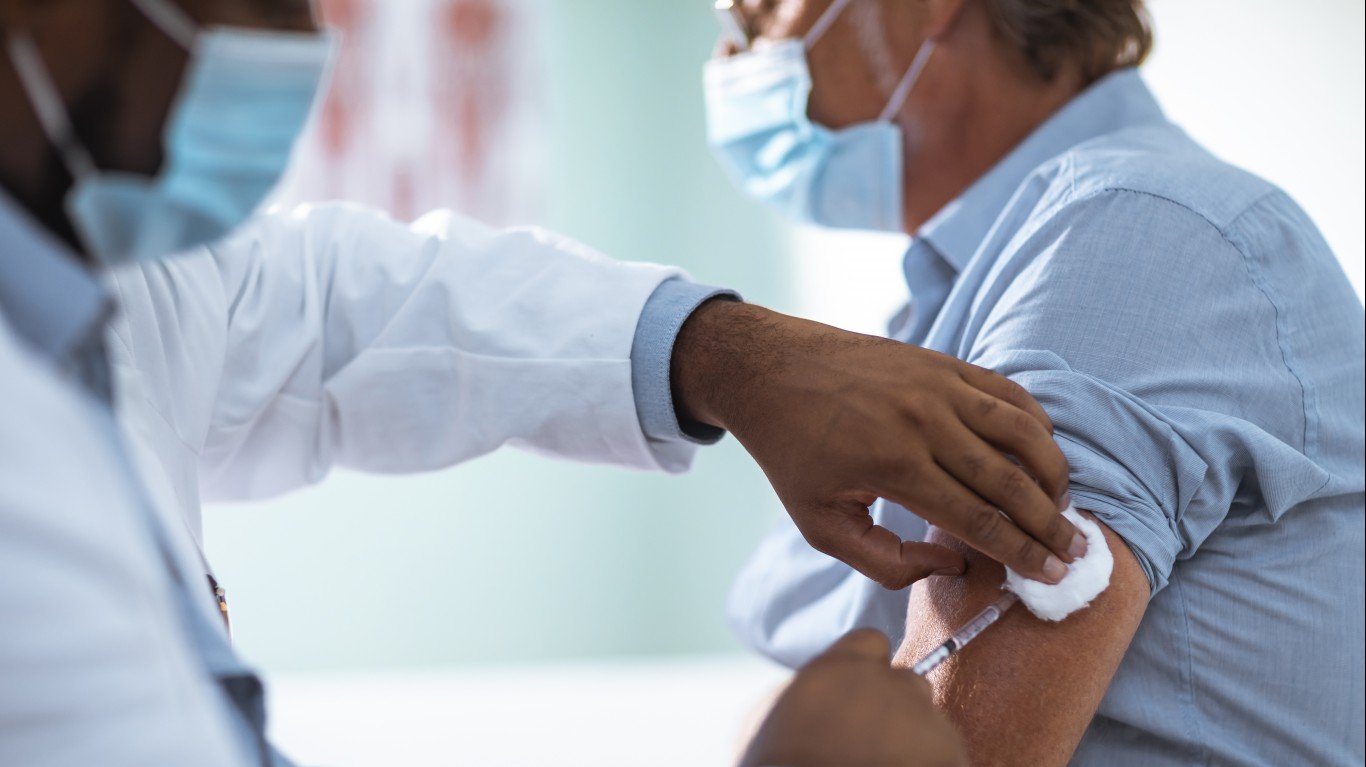
The U.S. has approved two vaccines, from Pfizer and Moderna. Another from Johnson & Johnson is likely to be approved within days. Nevertheless, the rollout of vaccines in America has been slow, particularly compared to other developed nations–especially the U.K. and Israel. About 14% of adults in the U.S. have received at least one dose. However, less than 7% have gotten two shots. At this point, 94,300,910 doses have been delivered in the U.S. and 70,454,064 shots have been given.
[nativounit]
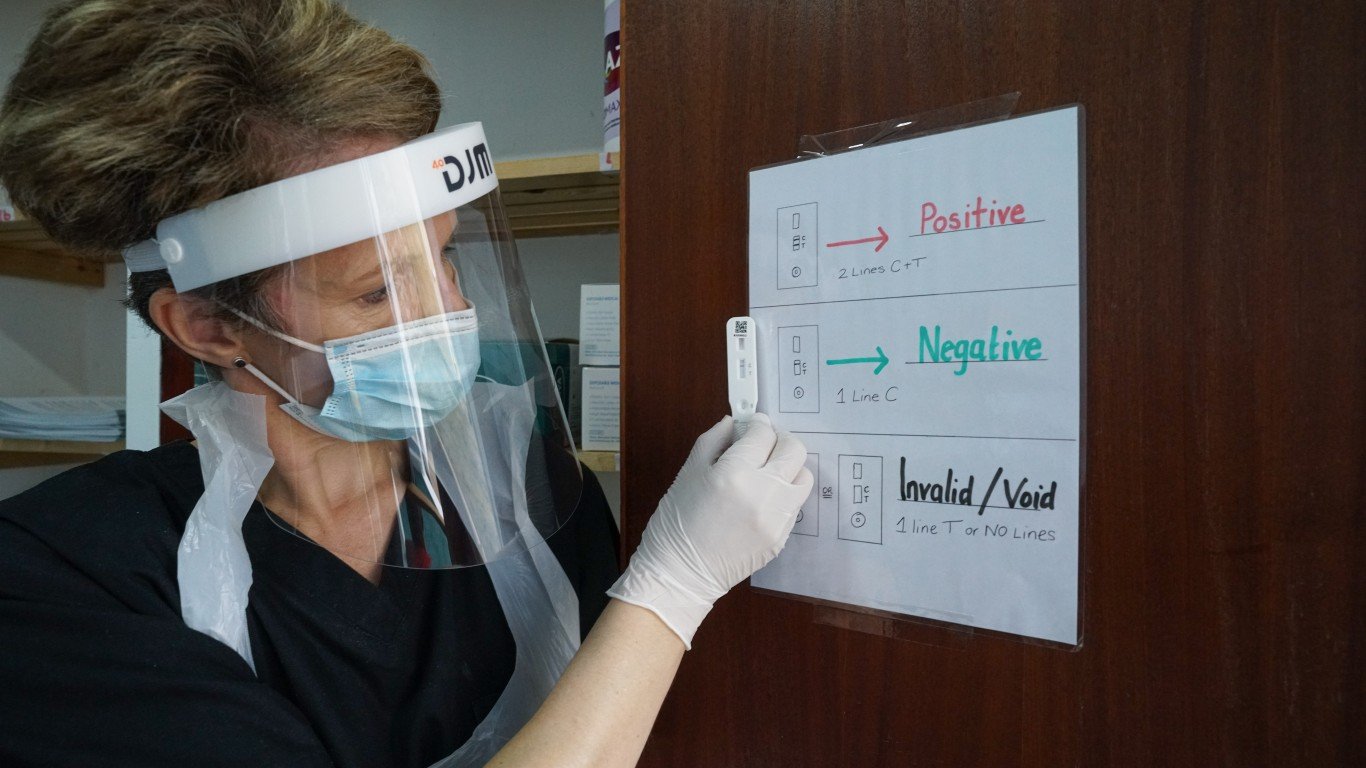
Testing and tracing in the U.S. have been criticized often, even if they have been improved over time. Actual cases in America have been put as high as 70 million, much more than double the official average. Much of that has been blamed on uneven rates of testing. And, testing remains critical to the ability to trace the disease–even if the spread has slowed.
Recently, the AP looked at testing rates and the trend was alarming according to several doctors. Dr. Clemens Hong, the chief of testing operations in Los Angeles County, the county with the most deaths among the nearly 3,100 in the U.S., said, “It’s shocking how quickly we’ve gone from moving at 100 miles an hour to about 25.” Testing locations in the county currently operate at only a third of capacity, according to the news agency.
The ability to do testing has become part of a battle for resources. Often, apparently, the personnel needed for testing are the same as those needed to give vaccinations. Dr. Jeffrey Engel of the Council of State and Territorial Epidemiologists told the AP, “You have to pick your battles here. Everyone would agree that if you have one public health nurse, you’re going to use that person for vaccination, not testing.”
Add concerns about testing to concerns about variants as reasons for another surge in the spread of the diseases. The CDC has identified three variants which it tracks and reports information on them to the public. Three have emerged on is public-facing radar scope. The most anxiety is over one from the U.K. which appears to spread rapidly.
Will vaccination rates beat low testing rates in the race to curb the disease? It should only take a few weeks to determine that.
Click here to read about the deadliest county in the deadliest state in America for COVID-19.
[wallst_email_signup]