

Doctors working in hospitals and emergency rooms have seen all kinds of infections and complications — from easily treatable urinary tract infections to potentially deadly sepsis. But some viruses scare them more than others, and they are more common than you think.
Most people probably fear human immunodeficiency virus (HIV), but in reality it’s not something doctors are frightened of, according to Dr. Paul Zelenetz, Chief of Division of Infectious Diseases at ProHEALTH Care. “It’s very rare,” he said. “Between 2000 and 2012, there was only one documented health care-related HIV acquisition.”
A lot of scary infections, such as Ebola, don’t spread that easily, but are made highly contagious because of lack of healthcare, noted Dr. Matthew Sims, director of Infectious Disease Research for Beaumont Hospital, Royal Oak, Michigan. “What makes it scary is where it’s spreading.”
What people in developed countries should be worried about the most are respiratory diseases because they can “really spread like fire,” Sims added. The other worrisome infections are those caused by bacteria that have become resistant due to overuse of antibiotics, according to Bonnie Prokesch, M.D., director of Antimicrobial Stewardship, Parkland Health & Hospital System and Assistant Professor of Infectious Diseases, UT Southwestern Medical Center.
Certain diseases are more likely to spread in hospitals because of the increased risk of accidental sticks with infected needles, and of breathing in an infectious virus or bacteria.
To identify the infections that even doctors find scary, 24/7 Wall St. consulted several doctors specializing in infectious diseases and reviewed prevention and treatment guidelines as well as death toll data from the Centers for Disease Control and Prevention (CDC) and the World Health Organization (WHO).
Click here to read about 10 infections even doctors are afraid of.

1. Flu
The scariest infection is the flu, according to Dr. Matthew Sims, director of Infectious Disease Research for Beaumont Hospital, Royal Oak, Michigan. “People think they are just going to get a little cough, but the flu kills 10,000 people in the United States in a good year.” The 2017-2018 flu season was the deadliest since tracking began in 1976, killing 80,000 people across the country.
“We have a vaccine that works very well, but it’s horribly underused,” Sims said. The virus “spreads like crazy” by coughing, sneezing, or even talking. Droplets can travel as far as six feet, landing on the mouths and noses of people nearby, infecting them.
One of the reasons why it spreads so quickly is that people are contagious 24 hours before they show any symptoms, Zelenetz, said.
[in-text-ad]
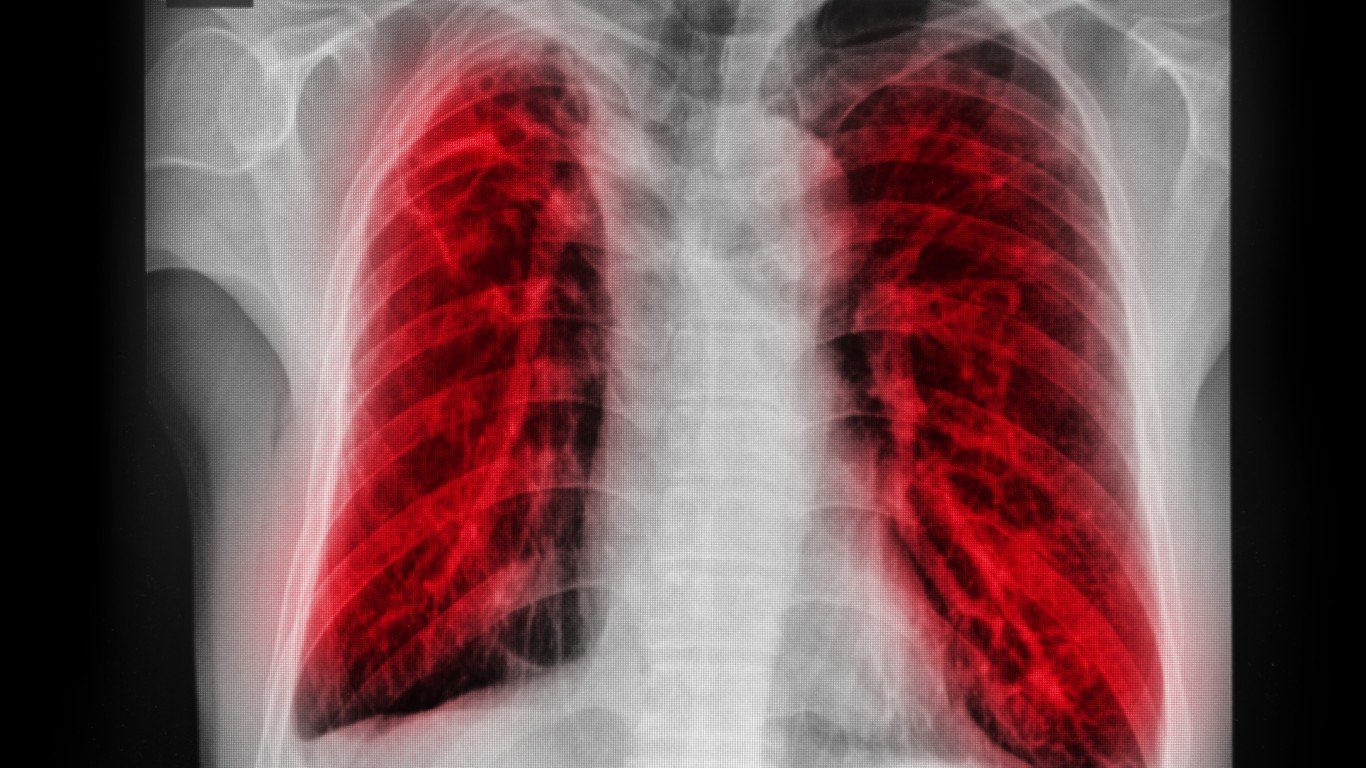
2. Tuberculosis
“After the flu, tuberculosis is the one I’d be most worried about,” Zelenetz said. The diagnosis is not always clear, and tests can be wrong. A weaker immune system can confuse the results. “The bacteria can float to quite a distance — you can be down the hall and still catch it,” he said.
The bacterial infection that mainly affects the lungs is airborne and can be fatal if left untreated. A person is no longer contagious after a few weeks of treatment, which can last up to a year.
Tuberculosis is among the top 10 killers worldwide, with more than 1.6 million people dying from it every year, according to the World Health Organization (WHO). Drug-resistant TB continues to be a public health problem; a recent report even suggested TB incidence may be on the rise.
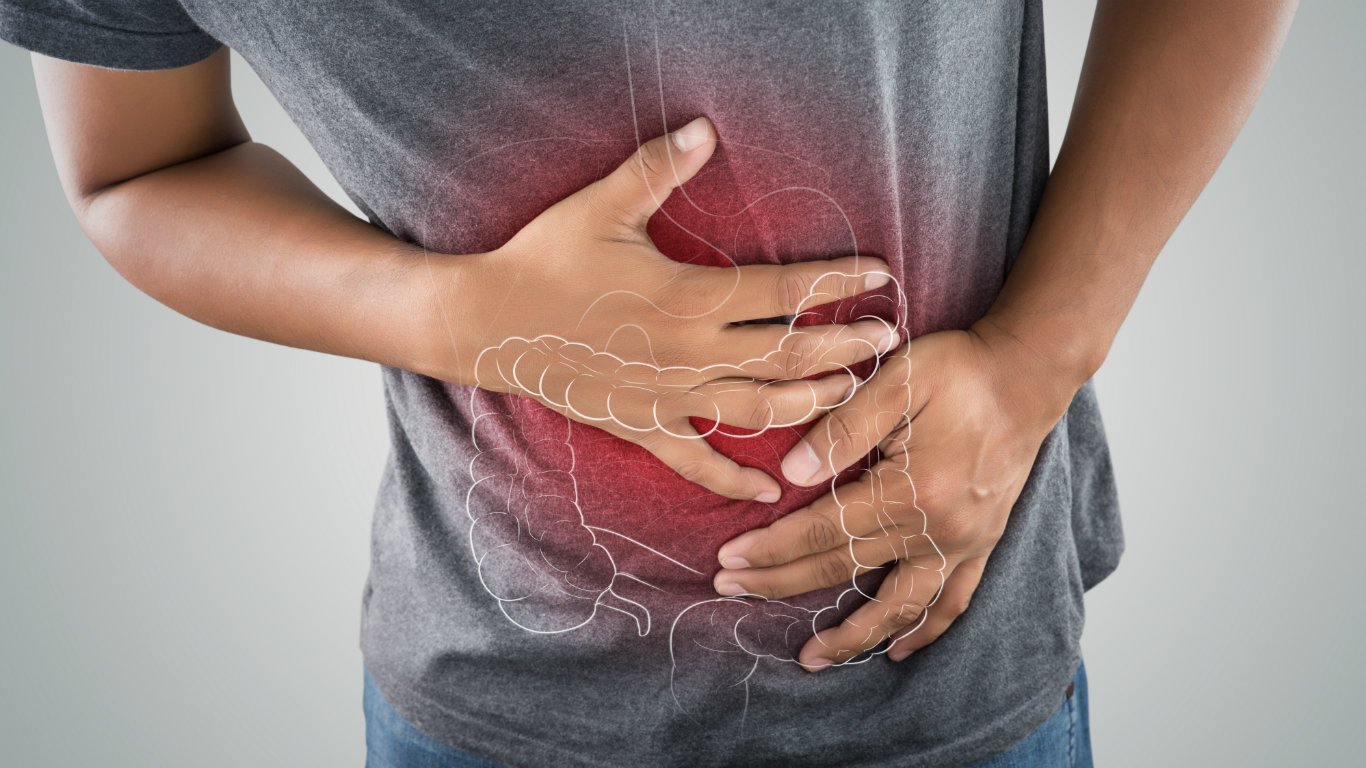
3. C. difficile
Clostridium difficile, usually called C. difficile, has become more common, Zelenetz said. The bacterium can cause diarrhea but also potentially lethal inflammation of the colon. About 500,000 people get infected a year, approximately 29,000 of whom die.
The infection is often spread in hospitals or nursing homes, where employees are more likely to catch it and spread to others. Older adults and anyone who has a history with the infection are at the highest risk, Sims said.
Patients can get infected after they are given antibiotics for something else. “People have the bacterium in their intestines but the good bacteria there keeps it under control,” Sims added. “Antibiotics kill that good bacteria, allowing for the C. difficile to grow.”
The best prevention method is thorough and frequent hand-washing. C. difficile spreads among people who touch any surface contaminated with feces, and then touch their mouths.
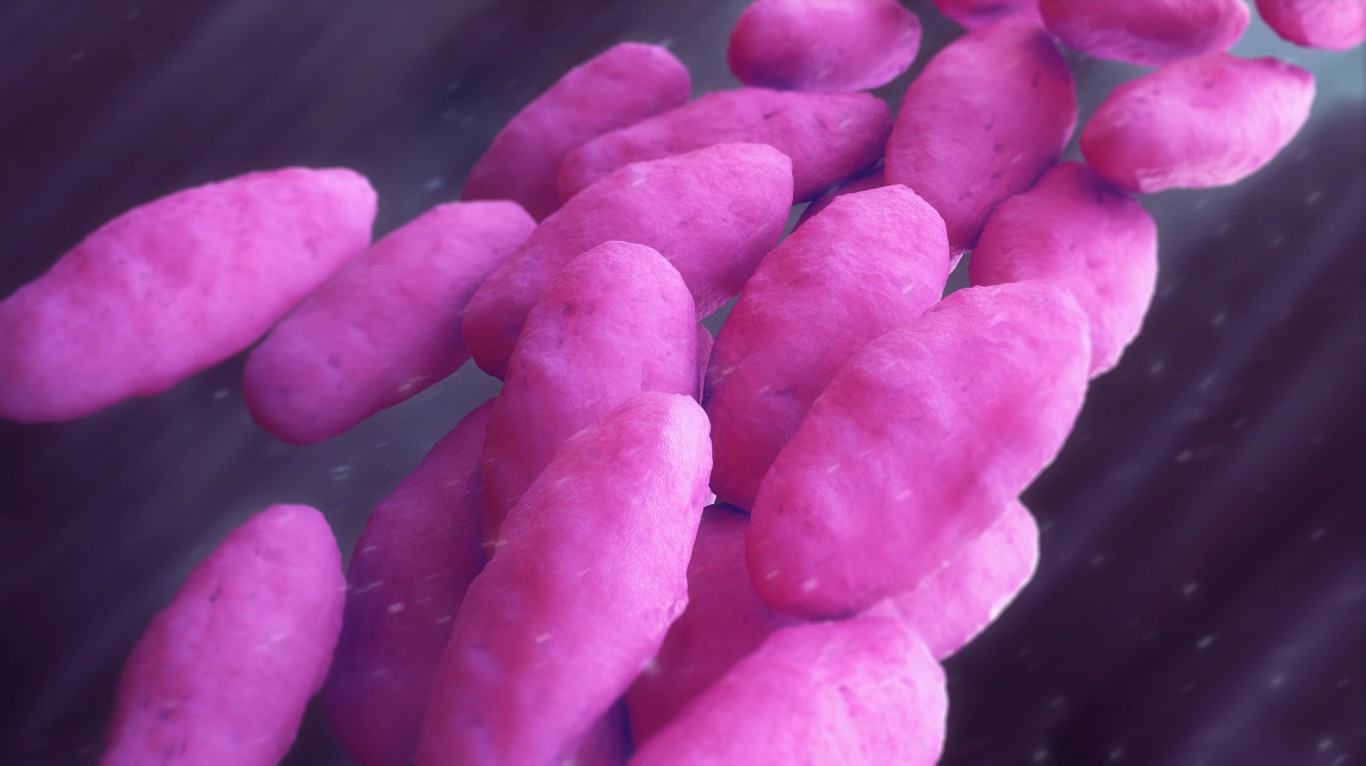
4. CRE
Carbapenem-resistant Enterobacteriaceae, or CRE, worry doctors because, as the name suggests, there are virtually no drugs to treat them, according to Zelenetz. They are highly resistant to treatment because they have an enzyme that breaks down the antibiotic, making it ineffective, Sims noted.
There are about 9,000 cases and 600 deaths a year. In some cases, the mortality rate is as high as 50%. People most at risk are patients in hospitals, who are taking long courses of antibiotics and need devices such as breathing machines or catheters.
CRE germs are usually spread through contact with infected people, particularly through contact with wounds or stool. They can enter the body through medical devices or wounds caused by injury or surgery.
[in-text-ad-2]

5. MRSA
Methicillin-resistant Staphylococcus aureus (MRSA) is an infection-causing bacterium that is difficult to treat due to its resistance to common antibiotics. “It can be more aggressive and needs special antibiotics,” Zelenetz said. MRSA can cause various problems ranging from skin to blood infections and sepsis.
In 2011, there were more than 80,000 invasive MRSA infections and over 11,000 deaths in the United States. Overall rates dropped 31% between 2005 and 2011. However, between 2000 and 2007, the number of kids hospitalized for infections due to MRSA more than doubled.
A person can get infected by touching infected skin or sharing personal items with a patient. Some of the symptoms include red and swollen skin bumps, rash, fever, and chills.

6. Viral pneumonia
“[Viral pneumonia] is transmissible just like the flu,” Prokesch said. “It doesn’t cause many problems in healthy people, but it can be extremely serious in immunocompromised people like kids, older people, patients undergoing chemo.”
Dozens of bacteria and viruses can cause pneumonia, including the flu or the common cold. Every year in the United States, about a million people seek hospital treatment for pneumonia, and 50,000 die. Vaccines are recommended for children under 2 and adults 65 and older, and for young people with certain medical conditions.
[in-text-ad]
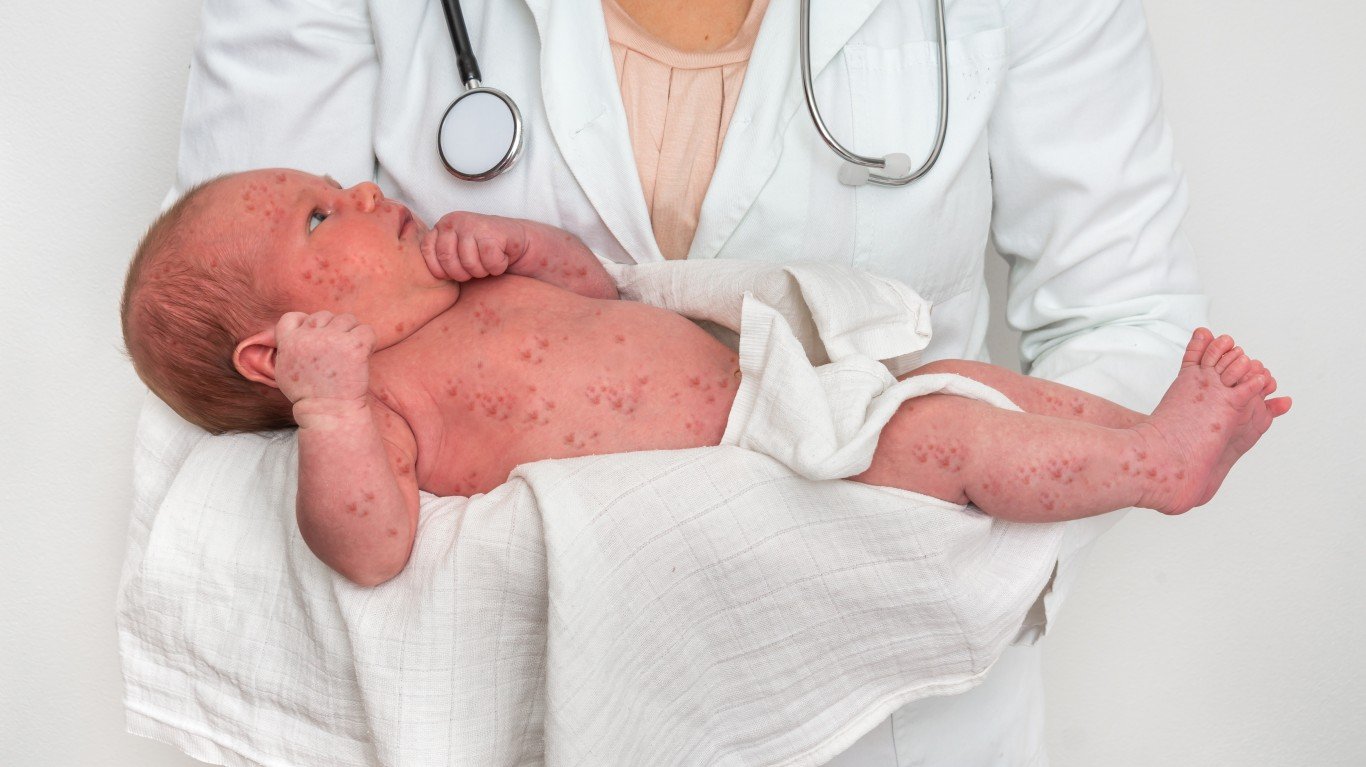
7. Measles
A recent measles outbreak across Europe and higher than usual reported cases in the United States have gotten some health professionals worried. There were more than 130 cases by October 2018, compared to 120 in all of last year. An outbreak in Rockland County, New York, alone reached 40 cases.
“The problem is that people are not vaccinating their kids,” Sims said. Measles was almost wiped out. It is now the deadliest vaccine-preventable infection, according to Prokesch. WHO calls it one of the world’s most contagious diseases. The airborne virus remains active on infected surfaces for up to two hours and can be spread up to four days before symptoms occur.
Children under 5 and adults over 20 are more likely to develop complications, including pneumonia and swelling of the brain, both of which can be lethal.
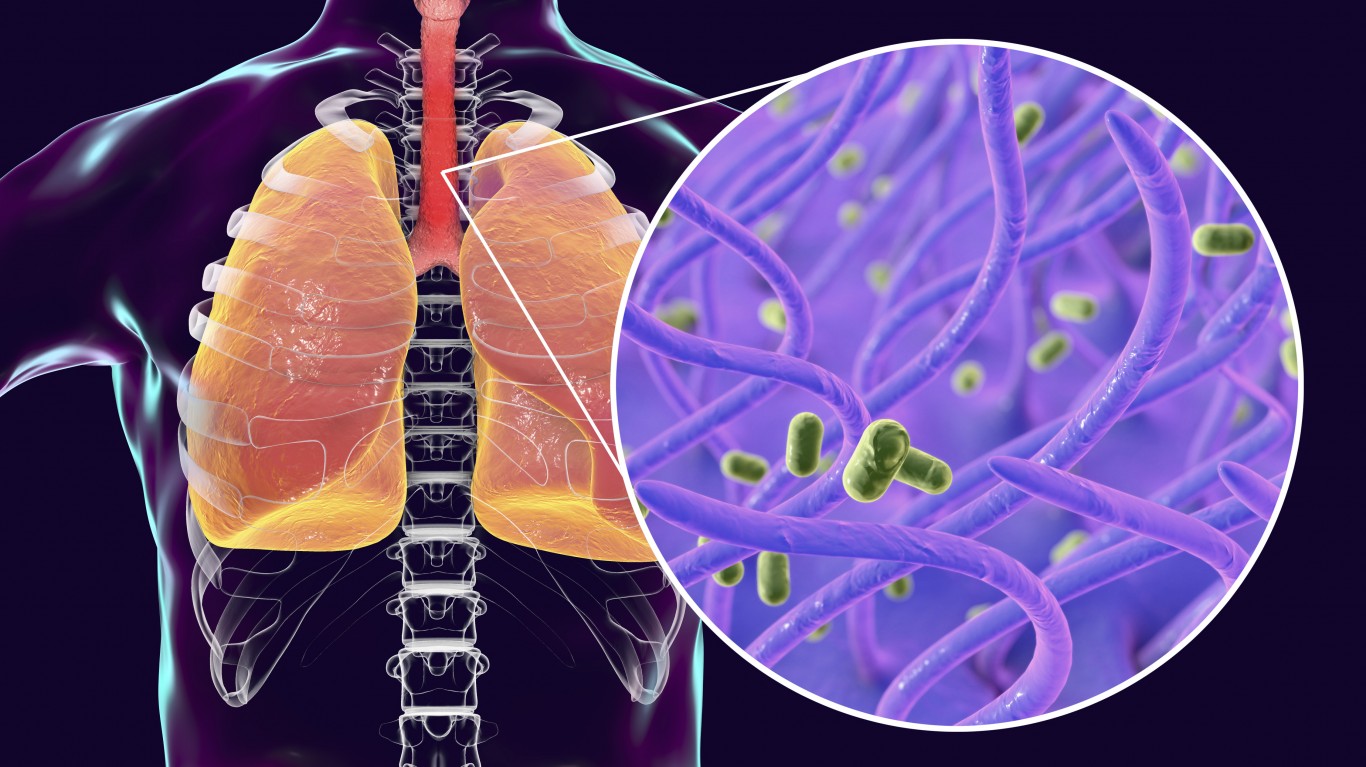
8. Whooping cough
Respiratory infections such as whooping cough, or pertussis, which is an infection in the lungs and breathing tubes, are easy to spread, according to Zelenetz. Anyone can get whooping cough, but it can be fatal for babies who have not completed the full course of vaccinations.
Half of those under 1 year old are hospitalized because they can suffer brain damage, have seizures or develop pneumonia. Other serious complications include vomiting, turning blue due to lack of oxygen, and difficulty breathing.
The CDC has reported an increase in the number of whooping cough cases, especially among teens and children between 7 and 10. “The vaccine works pretty well but it fades over time,” Sims said. “You should get it as a child and again as an adult.”
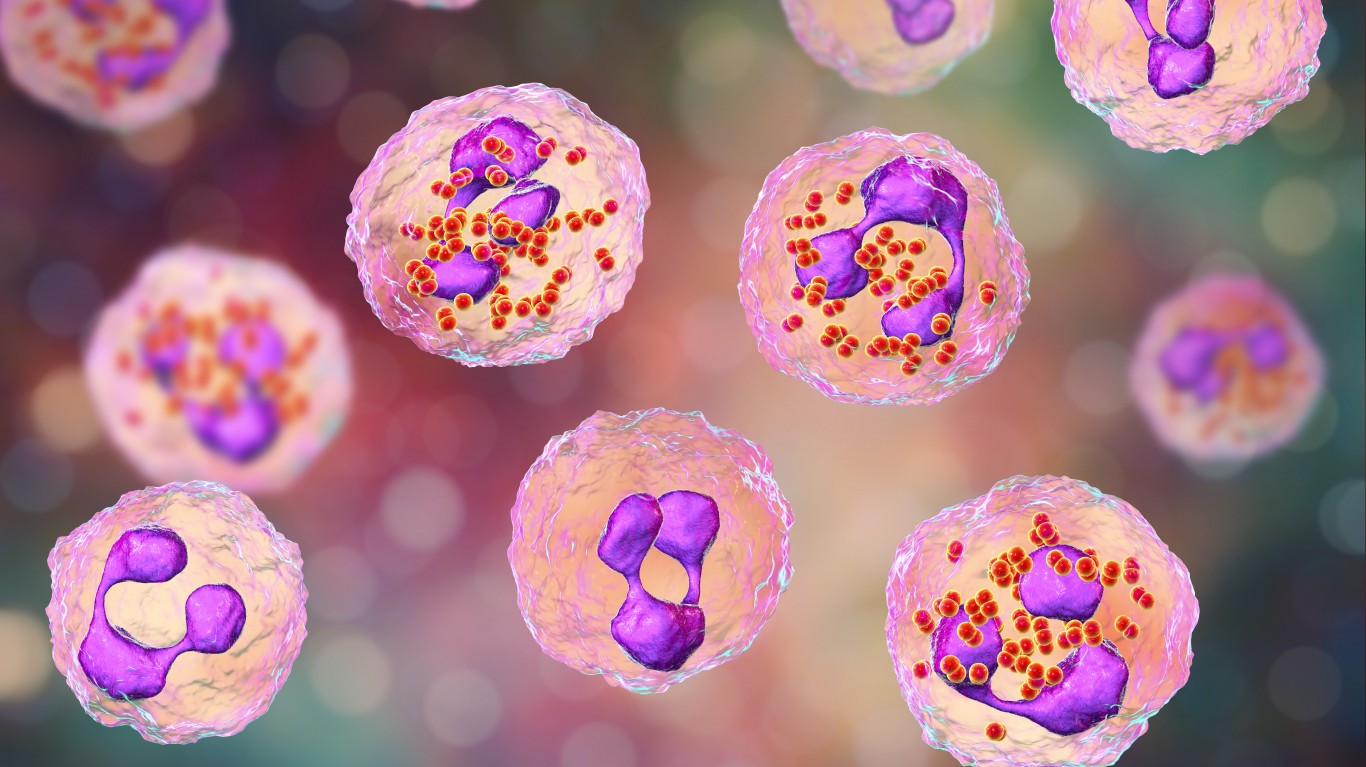
9. Meningitis
Meningitis, which is an inflammation of the brain and spinal cord caused by an infection, is a broad category. “The one that can be life-threatening and can progress very rapidly is meningococcus, “Zelenetz said. The bacteria can spread from person to person through very close contact, such as coughing on someone else or kissing.
Globally, 5% to 10% of those infected die, usually one to two days after the onset of symptoms. Meningococcus can be treated with antibiotics, but it has to be caught very early, according to Sims. The best way to prevent the disease is getting vaccinated. Vaccines are recommended for preteens, with a booster dose in young adulthood.
[in-text-ad-2]

10. Diarrhea
The viruses that can cause it is are highly infectious. Healthy people are not likely to experience complications, but in kids and people with suppressed immune systems infectious diarrhea can lead to dehydration and electrolyte imbalance, both of which can be dangerous, according to Prokesch. Diarrheal infections are very contagious because they can spread via dirty hands and contaminated food or water. All it takes is for one person to not wash their hands after going to the bathroom and prepare your food, Prokesch noted. “It all comes down to hygiene.”
Take This Retirement Quiz To Get Matched With A Financial Advisor (Sponsored)
Take the quiz below to get matched with a financial advisor today.
Each advisor has been vetted by SmartAsset and is held to a fiduciary standard to act in your best interests.
Here’s how it works:
1. Answer SmartAsset advisor match quiz
2. Review your pre-screened matches at your leisure. Check out the
advisors’ profiles.
3. Speak with advisors at no cost to you. Have an introductory call on the phone or introduction in person and choose whom to work with in the future
Take the retirement quiz right here.
Thank you for reading! Have some feedback for us?
Contact the 24/7 Wall St. editorial team.
 24/7 Wall St.
24/7 Wall St. 24/7 Wall St.
24/7 Wall St.
